For The Weekly Pulse (a revisit of an old Ms. column!), we’ve scoured the most trusted journalistic sources—and, of course, our Twitter feeds—to bring you this week’s most important news stories related to health and wellness.
In this edition of The Weekly Pulse, we rundown the most recent attacks to reproductive justice; address the presence of racial bias in health care; and provide updates on the coronavirus with a closer look at how exactly the pandemic is affecting mental health.
Repro Rundown
+ On Wednesday, the U.S Supreme Court issued a crushing blow to the reproductive rights movement by allowing employers to pose religious or moral objections to contraception. This decision upheld a predatory Trump administration rule that significantly stripped the Affordable Care Act’s requirement for free contraceptive coverage through most health care plans.
“We hold that the [Trump administration] had the authority to provide exemptions from the regulatory contraceptive requirements for employers with religious and conscientious objections, ” writes Justice Clarence Thomas for the majority opinion.
+ Abortion remains an important issue for voters, according to a Gallup Poll from May: 47 percent of respondents said abortion is one of the most important factors to their vote, and about a quarter said the candidate they vote for must share their views on abortion.
+ Liberal lawmakers and pro-abortion activists are disappointed after House Democrats decided to keep the Hyde amendment—which restricts federal funding for most abortion services since 1976—in tact in order to escape a partisan, pre-election clash.
“Abortion access is a right. That means it should not be available just to those who can afford it,” said Rep. Judy Chu (D-Calif.). “House Democrats have done more than ever before to protect the rights of all women, and I believe that should include the ultimate repeal of the Hyde Amendment.”
+ The National Institute for Reproductive Health’s annual “Gaining Ground” report assesses state efforts to advance reproductive health, rights and justice during the first six months of the year—during which time, 44 states and Washington D.C. introduced almost 550 bills to protect reproductive health care and access during the COVID-19 pandemic.
The health crisis has also “exacerbated and heightened the existing barriers to access to reproductive health care” for vulnerable communities, Andrea Miller, president of the institute, told ABC News.
Coronavirus Updates
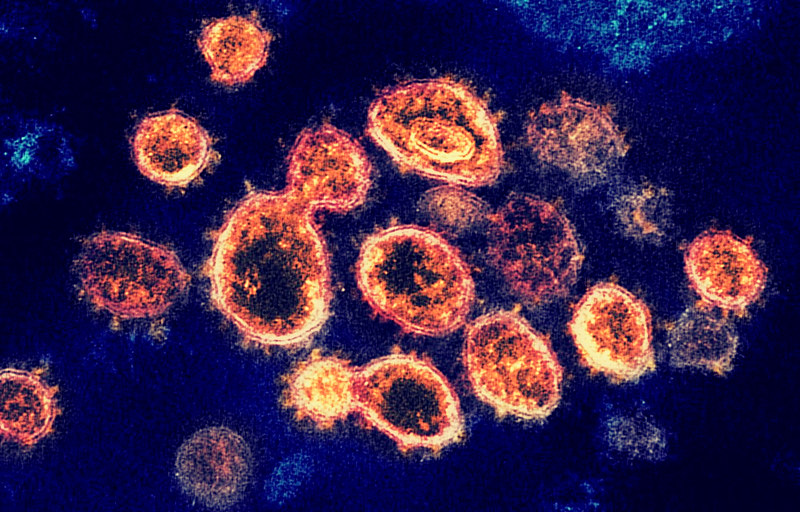
+ The federal government’s program to develop a COVID-19 vaccine, Operation Warp Speed (OWS), has so far invested four billion dollars into private companies. The goal of OWS is for 300 million Americans to receive a COVID-19 vaccine by January 2021.
This week, OWS invested $1.6 billion into the company Noravax to manufacture and administer 100 million vaccines by next year, assuming the vaccine proves to be safe and effective in on-going clinical trials. While the prospect of a vaccine coming soon is reassuring, some public interest groups are questioning the Trump administration’s lack of transparency in how spending decisions are made given that Noravax has never brought a product to market.
+ The pandemic is exacerbating existing inequalities through its disproportionate impact on vulnerable communities. In the U.S., a survey from the Urban Institute found the ripple effects of the pandemic are hitting those with low socioeconomic status the hardest. Similarly, data on the pandemic is showing COVID-19 hotspots in Europe are primarily developing in low-income areas.
+ Researchers are beginning to understand how COVID-19 may affect the body long term, including the brain. Brain inflammation, strokes, nerve damage and memory problems are among the symptoms noted in a U.K. study of 40 patients suffering from complications after recovering from COVID-19.
+ Neurologists are also closely monitoring COVID-19 patients who have since developed depression, preparing for the possibility that COVID-19 can cause issues with neurotransmitter levels down the line.
The Hidden Crisis: Americans’ Declining Mental Health
+ A report from the U.S. Census Bureau found one in three Americans are showing signs of anxiety or depression, which is a dramatic increase from the rates of anxiety and depression before the pandemic.
The psychological stress caused by the pandemic—such as financial stress, social isolation and fear about the virus—is likely to lead to the diagnosis of psychiatric disorders and other long term health consequences. Organizations like the National Institute of Mental Health are actively tracking the pandemic’s effects on people’s mental health.
+ Likewise, the coronavirus pandemic is causing opioid overdoses to skyrocket. According to experts, the pandemic is creating the social conditions that lead to “deaths of despair.” So far, 30 states have reported an increase in the rate of opioid-related deaths since the beginning of the pandemic.
Addressing Racial Bias in Medicine
+ As the nation continues to battle two pandemics—the coronavirus and racism—Black doctors are calling upon America’s health care system to combat and reduce systemic racism, bias and inequity. Advocates are calling for training on systemic racial bias in the medical field to be a required part of health care officials’ training in order to address racial disparities in treatment.
+ Under Executive Directive 2020-7, Michigan will require implicit bias training for health care professionals—a move recommended by the Michigan Coronavirus Task Force on Racial Disparities.
According to Michigan Governor Gretchen Whitmer:
“There’s no doubt that our front line health care workers like doctors and nurses have been the real heroes of this crisis, putting their lives on the line for us every day. COVID-19 has had a disparate impact on people of color due to a variety of factors, and we must do everything we can to address this disparity. The evidence shows that training in implicit bias can make a positive difference, so today we are taking action to help improve racial equity across Michigan’s health care system. That’s why my staff has begun this kind of training and every member of my team, including me, will complete this type of training on an annual basis.”





