Earning the trust of women is important in overcoming vaccine hesitancy and getting the entire U.S. vaccinated.
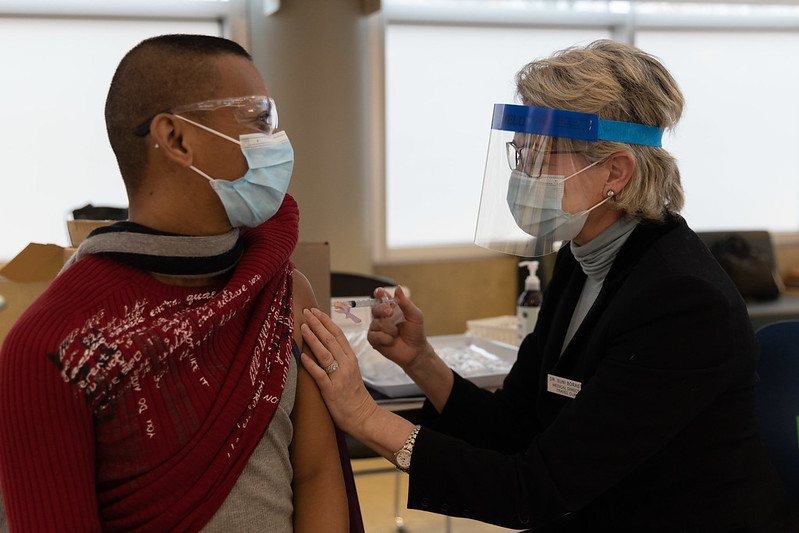
Women have been bearing the brunt of the COVID-19 crisis, from unequal caregiving and home-schooling responsibilities, to job loss. Women of color, in particular, are struggling: They have lost more jobs during the pandemic than any other group, and make up a large percentage of essential workers who cannot telework, increasing their collective exposure risk from the pandemic.
But although women are more likely to wear masks and follow social distancing rules, a concerning number of them report being wary of vaccinations compared with men.
In a December National Geographic survey, 69 percent of men surveyed said they were somewhat likely or very likely to take the vaccine, compared to 51 percent of women. Similarly, a Pew Survey found 45 percent of women, as opposed to 33 percent of men, would “probably not” or “definitely not” take a vaccine. And a January 2021 Kaiser Family Foundation survey found that over 60 percent of women are concerned that the COVID-19 vaccines are not as safe or effective as they are said to be, as opposed to 47 percent of men.
Earning the trust of these skeptical women will be essential in overcoming vaccine hesitancy and getting the whole population vaccinated.
Women: ‘Chief Medical Officers’ at Home
As women are responsible for most health care decisions for their household, including their kids and even their parents, this gender gap is particularly concerning.
- Seventy-five percent of mothers are the ones who take charge of health care responsibilities for their kids, compared to just only 20 percent of fathers.
- Fifty-nine percent of women make health care decisions for others.
- Moreover, 53-68 percent of women in the U.S. are caregivers, and over a third are caring for a parent or parent-in-law.
Combating COVID Misinformation
Because we are living through an unprecedented global pandemic, every rare reaction to COVID-19 vaccines have become fodder for national news—and inaccurate rumors about fertility risks and fear-mongering social media posts are fueling this fear. So-called “wellness” sites are propagating misinformation about COVID-19 in general, including COVID-19 vaccines. Women active on these sites (most of whom are white and upper middle class) mistakenly believe they have researched health issues when they utilize them.
Beyond the pandemic, too, the general lack of knowledge about health in our society must be addressed. For example, one study showed that although 53 percent of working women with kids under 18 believe “they are knowledgeable about keeping themselves and their loved ones healthy,” a mere 38 percent passed a health literacy quiz.
The “Warp Speed” Fear
Another worry about vaccinations are that they were developed too quickly. The Biden administration made a wise choice by dropping the previous administration’s moniker “Operation Warp Speed,” which hints at a rushed, frenzied process.
In truth, no steps were skipped. Over 40,000 people were in the clinical trials for the Pfizer-BioNTech and Moderna vaccines, the two currently authorized by the FDA.
The mRNA technology used in the vaccine has been developed since the 1990’s—not something that scientists came up with in a few months. Coronaviruses, like the one that causes the common cold, have been studied for decades.
A key way that the process was sped up was the government’s risky decision to provide funding for pharmaceutical companies to produce vaccinations at the same time clinical trials were ongoing. Those risks paid off: Both vaccines are over 90% effective—a rate experts call “exceptionally good.”
The Pregnancy Conundrum
Additionally, there is a real concern that pregnant people were not included in the COVID-19 clinical trials. Unfortunately, the exclusion of pregnant women is common: Almost three out of four drugs approved by the FDA since 2000 did not include any pregnancy data at all. The World Health Organization has noted that animal studies show no harmful effects of these mRNA vaccines on pregnancy, but that due to the current lack of data in pregnant women, they recommend vaccinations of pregnant women when “the benefit of vaccinating a pregnant woman outweighs the potential vaccine risks.”
The American College of Obstetricians and Gynecologists notes that the vaccines should not be withheld from “pregnant individuals who meet criteria for vaccination.” COVID-19 infection poses serious risks for those who are pregnant and their infants. Conversely, emerging data published in the Journal of the American Medical Association’s JAMA Pediatrics suggests pregnant women may pass on antibodies to their baby in utero—a case for vaccination.
Pregnant people who may be exposed to infection, such as essential workers, should be given correct, accessible information to address their fears about the vaccine.
Public Health Messaging is Key
We need to make sure women receive accurate vaccination information easily. Julia Marcus, an epidemiologist at Harvard Medical School, suggests that narrative around the vaccine should emphasize its efficacy and safety. The federal government needs to fund massive public health campaigns to help educate the public about the vaccines, dispelling myths about mRNA technology (like the false claim that it “alters” one’s DNA or causes infertility). In truth, the risks of getting infected with COVID-19 are much greater than the risks of vaccination.
Public health messaging should be tailored to women and to Black, Latino, and Indigenous communities—groups with the highest rates of vaccine hesitancy. Having President Biden getting a vaccine on television may not be as effective in changing minds as having trusted female community leaders and physicians deliver this message, addressing concerns specific to women. The messaging should be delivered in ways that are accessible, such as with text messaging, social media campaigns, and in multiple languages.
Ramp up Number of Vaccines and Access to Vaccines
The vaccine rollout has been haphazard and uncoordinated, with access to vaccines varying based on internet speed, technological knowhow, and zip code. The government and public health officials need to quickly address both vaccine access and hesitancy. If women and people of color are already skeptical of the vaccine due to historically justified mistrust and mistreatment by the medical system, there need to be sincere efforts to gain trust by providing honest, clear, consistent information about the vaccines.
We need more COVID-19 vaccines, more vaccination sites in more varied areas, and easier access to vaccine appointments. If one is on the fence about getting the vaccine, they will not stand in line or get online in the middle of the night to get an appointment. Studies show if you know someone who has gotten the vaccine, you are more likely to get it yourself.
A combination of better information and messaging and greater access will help combat vaccine misinformation and hesitancy in women.
You may also like:





