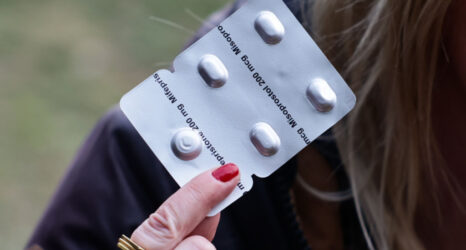
As the Supreme Court threatens to overturn abortion rights, expanding access to emergency contraception to prevent unwanted pregnancy is more important than ever. This student-led peer group is making it happen.

For years feminists waged a hard-fought campaign to make emergency contraception (EC) available over-the-counter for everyone. They succeeded in 2013, but college students still face many barriers.
EC can cost up to $50 and needs to be taken quickly, within three to five days of unprotected sex. Getting EC when you need it can be a challenge because health centers and pharmacies have limited hours, especially on nights and weekends when people need EC the most. Buying EC can be daunting for young people because it’s not always stocked directly on the shelf, forcing them to ask a pharmacist for the medication, which can feel like an invasion of privacy, especially in cases of sexual assault. Many states allow pharmacists to refuse to dispense EC if they have moral objections.
To address these barriers and others, advocates are organizing to increase awareness about EC and ensure quicker, easier and more private and affordable access to EC on college campuses.
The American Society for Emergency Contraception (ASEC) has created a campaign called Emergency Contraception for Every Campus—known as EC4EC—to mobilize and assist students to develop peer-to-peer EC distribution networks on college campuses and to advocate for EC vending machines.
“I am committed to doing this work because over the years that I’ve spent working on EC, I see how difficult it can be for people to access it,” Kelly Cleland, ASEC executive director, told Ms. “It’s incredibly important to get EC as soon as possible to increase the chance that it’s going to work. We really need to get rid of barriers. And when we see the barriers that young people in particular face in terms of being asked for ID when they get to the pharmacy, in terms of the stigma and judgment that they received some times, it’s just unconscionable.”
“When we see the barriers that young people in particular face in terms of being asked for ID when they get to the pharmacy, in terms of the stigma and judgment that they received some times, it’s just unconscionable.”
EC prevents or delays ovulation—release of an egg from the ovary—so there’s nothing for sperm to fertilize and pregnancy can’t occur. Emergency contraception is different from the abortion pill. EC prevents pregnancy before it occurs and will not end an existing pregnancy.
There are two types of dedicated EC pills: progestin-only and ulipristal acetate. The brand name progestin-only emergency contraception—Plan B One-Step—is now available over the counter in every state with no restrictions on the age or gender of a person buying it. The progestin-only pill is also available in several generic forms, including Take Action, Aftera and AfterPill.
The second type of EC—ulipristal acetate—sold as Ella, requires a prescription. This form is typically more effective, particularly for those who weigh more than 165 pounds.
Cleland says there are many barriers for college students seeking access to EC. “I think a lot of people don’t know that Plan B exists. They don’t know that there is actually a more effective option, which is the prescription-only form of EC, Ella. I think about just the timing and people not realizing you need to pick it as soon as you can.”
“In terms of other barriers is logistics,” she continued. “Where is the pharmacy? Do they even have it in stock? If you’re on a college campus, does your student health service have it? Then does your insurance cover it? And then there’s the question of, if you weigh more than 165 pounds, is this going to work? Can you get the more effective option? There are a lot of complex factors that come into play.”
The American College Health Association’s 2019 survey revealed that 27.5 percent of student health centers do not provide Plan B, 35 percent of centers do not prescribe Ella, and 55 percent do not dispense Ella. While most schools provide EC information to students, 12.4 percent do not even do that.
Cost can also be a significant barrier. Pharmacy prices are high—$40–50 for Plan B One-Step. While less-expensive generic versions are available online for a little as $7.99 plus shipping, delivery times may be too slow.
To address these barriers on campus, ASEC created EC4EC with an advisory board of young people from around the country, who do outreach to other students and respond to requests for information about how to develop services on their campuses.
EC4EC offers a toolkit, a step-by-step guide on how to increase access to EC on campus, including who to talk to, how to find allies, what some of the logistical considerations are, and how to build support. After consulting with a new student organizer, EC4EC provides them with supplies, including 20 doses of EC, 50 condoms, 20 pregnancy tests, and information pamphlets to distribute.
“Students are really stepping up and providing care for each other and putting systems in place for each other,” said Cleland. “I think it’s just incredible.”
Peer-to-Peer Networks
One of those students is Jo Morganelli, who organized a peer-to-peer distribution network with about 30 volunteers to answer a hotline and deliver free EC to students at Towson University in Maryland. Morganelli says the network helps students overcome barriers to EC, such as limited hours at the health center, which is only open Monday through Fridays from 8 a.m. to 5 p.m.
“When are college students going to need EC most likely? On the weekends, when we’re not in class and we’re going out. If you have unprotected sex on a Friday night, if you don’t get an appointment at the health center on that Monday, then you’ll have to get a prescription to take another medication.”
Morganelli spoke to the panic that students feel when they need EC and don’t know how or where they can get it or how they can afford it.
“I’m glad that we were able to serve so many students and help them alleviate that panic and that stress of being 18 and having no money. Not being able to know if you can afford Plan B. And now all of a sudden having to worry about how you’re going to afford to raise a kid or have an abortion or take off work to go get EC. Do you have to ask your parents? How are you going to deal with that? It’s a kind of panic that is hard to explain. It feels like everything is out of your control.”

Morangelli says the privacy of the service was particularly appealing to students.
“When we first started the hotline, we did surveys asking why you’re using the service, have you gotten EC before, what was your experience like,” said Morganelli. “Almost across the board everyone was like, ‘I am ashamed, I feel shame, or I don’t even want to go and make the appointment at the health center because then the doctor will know, or then my parents may find out because it’s on my insurance.’ There’s a lot of shame and stigma.”
Morganelli shared her own experiences of feeling stigma when purchasing EC. “Both of the times I had to purchase Plan B, I remember the looks that I got from the cashiers. I remember them checking my ID and saying snide comments and how that affected me. They didn’t have to check my ID, but I didn’t know that.”
Privacy is a concern as well for students at Hampton University, an HBCU in Virginia, where rising senior Amber Wynne runs the repro hotline that distributes EC as well condoms, dental dams, pregnancy tests, pads and tampons. They offer confidential and contactless delivery by mail or drop off.

“There’s a distrust between the students and the university,” said Wynne. “They prefer to come to us rather than the health center. I would definitely feel more comfortable going to a student who has these resources, one for free, but two, who is not going to make you feel judged. We’re more focused on helping you make it to tomorrow, rather than making you feel scrutinized for the reason you’re seeing us. Whatever the reason, we don’t care. We just want to make sure you’re okay. I have had students come to me and say that the health center told them, ‘Do you want to pray on it?’ and ‘Why didn’t you put on a condom?’”
Wynne says that students are often suspicious of the health care system. “Historically, when we look at how the reproductive health care system has oppressed Black people, I can’t blame students for not having an ob-gyn or going to the doctor when they have a reproductive health care concern because what we’re hearing is family members who have had their uteruses taken out or you have a family member who’s been sterilized without their consent. It’s very scary and very traumatizing. One thing I actually had a student tell me a couple weeks ago was that the fact that you look like me and that you’re my age and you understand what I’m going through, that means everything.”
“I actually had a student tell me a couple weeks ago was that the fact that you look like me and that you’re my age and you understand what I’m going through, that means everything.”
The repro hotline also provides educational resources. “At Hampton, since it’s an HCBU, 95 percent of the students look like me. We’re not getting the birds and the bees talks about emergency contraception and condoms,” said Wynne. “Those aren’t conversations we’re having at our dining tables.”
EC Vending Machines
In addition to peer-to-peer networks, EC4EC works with students to put EC vending machines on college campuses.
Parteek Singh campaigned for two years to get an EC vending machine at UC Davis. He succeeded during his senior year in 2017. The machine is accessible 18 hours a day and “doesn’t give judgmental looks,” said Singh.
“The stigma around sexual health is a barrier. That’s one of the big things that the EC vending machine does. It removes the human interaction, which in itself is increasing accessibility. People still don’t feel comfortable talking about sex and sexual health. There is just not enough conversation where it’s normalized. And most people are buying it for the first time.”
Singh says these barriers are particularly hard for students of color. “When you talk about API communities or POC communities, there is even less talk of sexual health. I think there’s more judgmental looks there. Some cultures don’t approve of sex before marriage, so there are those cultural barriers as well. So the machine is breaking all those barriers.”
The vending machine at UC Davis sells a range of over-the-counter health and wellness products to serve the whole student body and ensure privacy for people purchasing EC, says Singh.
Singh graduated in 2017, but he still advises students interested in setting up an EC vending machine on their campuses about how to do it, including assessing what resources are available, surveying students about what they need and want, and negotiating with college staff to get it done.
Morganelli also looked into creating vending machines for EC on campus, but Maryland at the time was one of a few states that prohibited them. She worked with Maryland NARAL to change the law, which happened last month.
“Besides just improving access for people, I think the law will also help reduce stigma because it’s making it more regular,” said Morganelli. “If you look at a vending machine and you see you got your pens, your pencils, and notepads, some EC, some condoms … then it’s going to be less stigmatizing.”
Morganelli, Wynne and Singh serve on the student advisory board of EC4EC, working with students around the country to set up EC access on their campuses.
Making EC Accessible on Every Corner
EC4EC is connected with students on 55 campuses, says Cleland. Fifteen campuses in seven states now have EC vending machines, and more campuses have peer-to-peer networks.
ASEC regularly issues an EC access report and has fact sheets, including EC and COVID and EC and transgender health care. Cleland says ASEC is currently conducting a new survey this summer to better understand students’ knowledge about EC and the access situation on and around their campuses.
“I feel like we need people to do whatever they can to help people get it, especially young people, as soon as they need it,” said Cleland. “We see on some of these campuses, the student health service doesn’t provide it, they may be in a rural area, students may not have a car, they may not have the money to get it. I want to do everything I can to help students support each other in getting this time-sensitive care.”
ASEC recommends that people at risk of pregnancy keep EC on hand in advance of need.
“This is a method that’s gone basically from nobody having known much about it in the 1990s to now over-the-counter access, which is great, but still not enough people know about it as an option when they need it,” said Elisa Wells, co-director of Plan C and one of the advocates who fought for over-the-counter access to EC. “So any effort to increase visibility of the methods is obviously really important and having the convenience of an on-campus, immediate solution through vending machines is fantastic.”
As the Supreme Court threatens to overturn abortion rights in the U.S., expanding access to EC to prevent unwanted pregnancy is more important than ever.
“I hope there are EC vending machines everywhere, and not just on college campuses,” said Morganelli. “I want them in communities, in bodegas on the corner, in CVS, in just random parks around the city. And in family planning deserts.”
For more information about how to increase EC access, contact Kelly Cleland at ec4ec.org/contact/ ASEC’s newsletter here.
Up next: