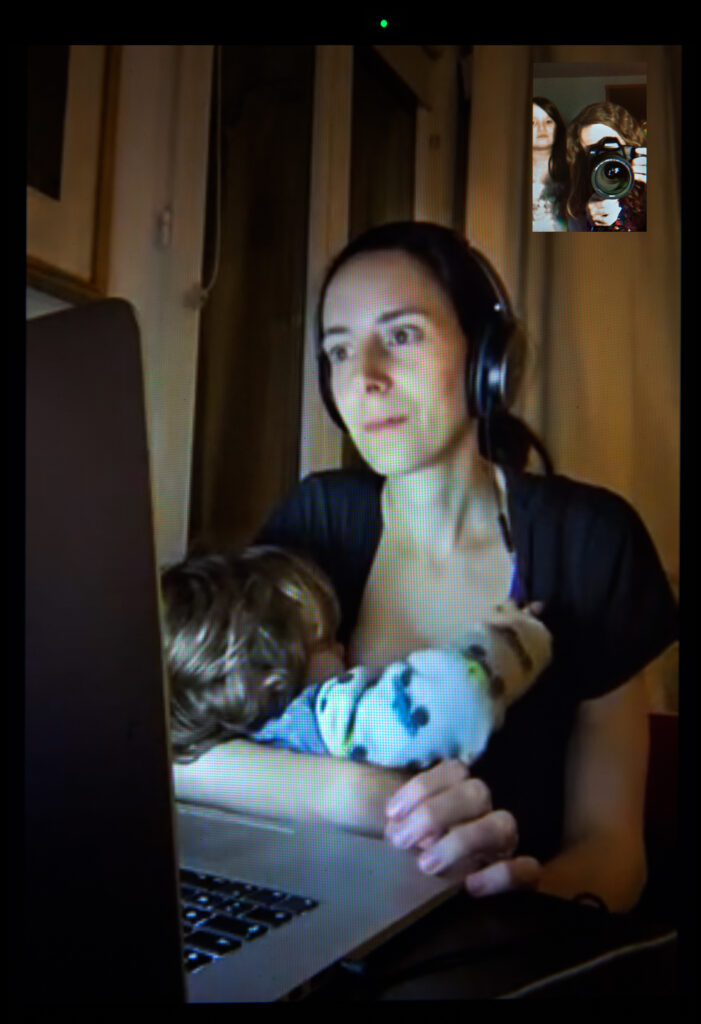
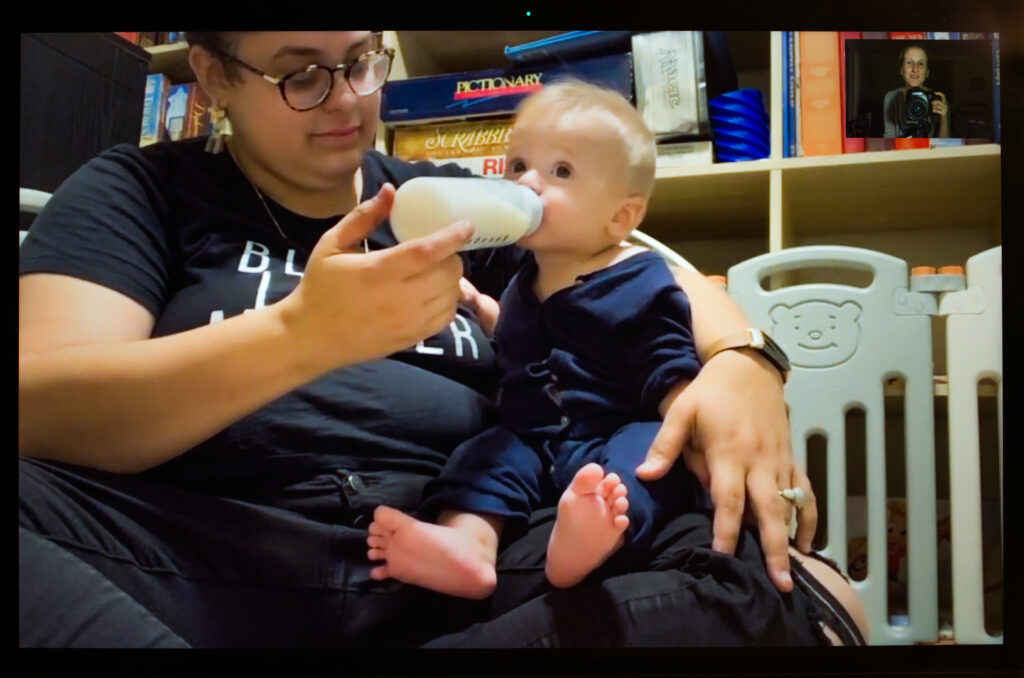
If the 2000s were the decade of the “brelfie”—carefully curated breastfeeding selfies posted on social media—2020 could be dubbed the year of “laczoom,” to connote the different ways in which people expose their lactation online.
I was recently preparing to sign on to an online faculty meeting, when my two-year old began to scream, “Tétée! Tétée!”—the French for “boob” and “suckling”—thirty seconds before start time.
With little time to think, I hit “Join Meeting,” put him on the breast, and attempted a smile. But wait—should I turn the camera off? As a legal scholar who writes about lactation as an under-recognized and unrewarded form of gendered labor, I could not possibly turn it off. I noticed that there were 50 participants on the call. Would I come across as unprofessional? Or just French? Keep the camera on, I told myself.
It was a bit scary. Uncomfortable. But I’m tenured. I’m a white, cishet woman who is privileged in many ways—the type of person who ought to use her position to make lactating labor more visible.
A couple of minutes in, a senior colleague texted me, “Are you nursing?” I wrote back, trying to project confidence, “Of course! Online public nursing, my current research topic.”
If the 2000s were the decade of the “brelfie,” that is, of carefully curated breastfeeding selfies posted on social media, 2020 could be dubbed the year of “laczoom” to connote the different ways in which people expose their lactation online. Unlike brelfies, which risk censorship on Facebook or Instagram if they violate indecency and nudity policies, laczoom happens in real time, reducing the chance that it will be blocked.
Nevertheless, much like breastfeeding out in the world is expected to be low profile—a few state laws actually require discretion—nursing online is tolerated when not too conspicuous. A woman who kept her mic and camera on while breastfeeding during a work meeting was recently shamed on Reddit by a coworker.
The pandemic and its accompanying turn to online spaces for work, socializing, education, health xcare and more, exposes the contested nature of breastfeeding as an activity many view as private when it is a matter of public importance implicating the renewal and well-being of our polity, species, other species and the environment. At the same time, the crisis challenges the public-private divide itself by transforming the home into a semi-public space through video-enabled devices.
Lactation has become simultaneously more and less visible. In the age of social distancing, nursing in public is waning from our collective sight. At the same time, a novel form of public lactation is developing online, in particular on videoconferencing platforms, which function in many ways as the new public space.
Visual artist Corinne Botz and I teamed up in April to explore this question with the goal of making parents’ infant feeding labor and experiences more knowable and visible. We connected with over thirty parents and lactation professionals.
Botz, who previously photographed lactation rooms in the workplace, was now holding virtual photo shoots using her camera and laptop to photograph in homes across the country. Botz moved with participants around their houses, guiding them on where and how to set up their device for the photographs, listening to good-night stories, meeting family members, witnessing breakfast leftovers and toys strewn on the floors. This is photography in the time of social distancing.
The pandemic makes it harder for many new parents, especially the most vulnerable and marginalized, to initiate and maintain their lactation. They are isolated, have diminished access to in-person lactation counseling and may suffer from economic hardship and illness. They may also work stressful shifts as essential workers.
Lactation can be particularly fraught for Black and Indigenous women, whose reproductive and lactating labor has historically been exploited for white interests. The COVID-19 outbreak has amplified racial disparities in maternal health and breastfeeding rates. During the first months of the pandemic, hospital restrictions on birth and breastfeeding, such as the separation of COVID-positive or COVID-suspected parents from their newborns, disproportionately affected Black and Indigenous women, reviving the history and trauma of separating enslaved and native children from their mothers.
At the same time, the coronavirus has worked as a breastfeeding campaign of sorts. Camie Goldhammer, a Sisseton-Wahpeton lactation consultant and founder of the Indigenous Breastfeeding Counselor training, reports, “lots of people … really wish that they were breastfeeding” for the immunological benefits it could confer. For some parents, the pandemic has been a catalyst for producing more milk. Alarmed by reports of infant formula shortages, Black breastfeeding specialist Nichelle Clark went as far as relactating to provide her son with milk and donate the surplus through her social circle and the Facebook group she co-founded, Breastmilk Donation for Black Mothers.
Other women ended up with a stash of frozen milk, which they did not need because they were not leaving their houses. Britta Fithian-Zurn, a white graphic designer from Oregon recounts, “I had built up this supply thinking I would go back to the office, and it was taking over our freezer. The first donation was 200 ounces or something.”
Around the nation, human milk banks have been flooded with donations. Desiree Joy Frias, a queer Afro-Latina woman and community activist, had to quit breastfeeding. But she received thousands of free ounces of donor milk from families she found online. “It’s nuts. I feel like a cat burglar packing up three coolers with all that breast milk.”
Back in 2015, anthropologist Penny van Esterik asked, “What would happen if human milk were really treated like liquid gold? What accommodations would be made for it and for its producers?”
Five years later, even during a pandemic, parents who produce this valuable resource too often continue to be unseen and unrewarded. Veronica White is a Black critical care nurse in Michigan and mother of two. “Because of the pandemic and everything, we’re really short-staffed,” she notes, “so there is no way I could get away four times during my shift to pump.”
To maintain her lactation, she purchased a $500 high-tech wearable pump allowing her to express milk during her shifts unbeknownst to most of her patients and colleagues. She saves lives but must lactate furtively.
It remains to be seen whether the emergence of videoconferencing apps as our new pandemic public space will contribute to normalizing nursing in public or further consign it to the private sphere. There are similarities here with the increased availability of lactation rooms and pods in the workplace and in public or semi-public spaces. This development has been applauded as providing a welcome alternative to nursing or pumping in bathroom stalls. But what is the message sent by these facilities (or the possibility to turn off cameras and mics)? Is it, “We support you and your infant feeding choice” or, “This activity should be concealed”?
One lesson of the COVID-19 crisis for policy and lawmakers may be that to adequately support lactation, they should take cues from the families who had positive experiences in conditions of quarantine. These are typically the well-resourced parents not working outside the home or telecommuting and who have help from their partner and others around them. They have the opportunity to engage in practices known to support lactation such as increased time at home, rest and access to breastfeeding support. In some ways, they observe traditional postpartum customs and rituals known in some cultures as confinement—which incidentally is a term also used to denote quarantine.
For all new parents to experience their preferred version of postpartum confinement, here are some of the legal and policy tools which should be available: family-centered pre- and postpartum care, universal basic income, paid parental leave, paid lactation leaves and breaks, a flexible work environment, affordable housing, universal health care and equal access to high-quality, non-discriminatory and culturally appropriate care (including lactation counseling), and sliding fee child care programs.
You may also like: