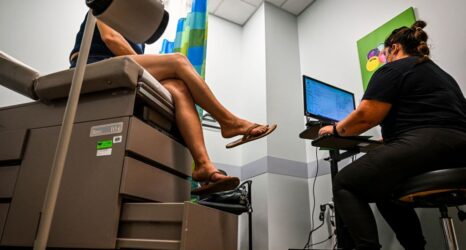
As the pandemic rages on, the role of nursing staff has been frequently overlooked and consistently undervalued.

In a recent headline, CNN alerted the public that health experts may “begin rationing nurses, equipment and care.” This messaging minimizes the expertise and skill that a nurse provides to hospitalized patients by aligning nurses with equipment and hospital beds.
Throughout the COVID-19 pandemic, media outlets and government officials have reported the shortage of hospital beds throughout the country. In response to increasing demand for hospital beds, hospitals have added additional beds, shifted resources and stockpiled supplies.
Yet while focusing on “supplies” such as ventilators, medication, oxygen and “space” (e.g., number of beds, hospital capacity)—the role of nursing staff has been frequently overlooked and consistently undervalued. Headlines that focus on physical resources miss two vital components of critical care:
- a hospital bed is just that—a bed—without a skilled nurse providing care to the patient in it, and
- a competent critical care nurse cannot be produced on demand.
Nurses undergo extensive education and specialty training that enables them to care for the sickest of the sick. To care for critically ill patients, such as those with respiratory failure from COVID-19, nurses must have extensive knowledge of human physiology and the ability to assess for impending deterioration and complications of therapies. Nurses working in Intensive Care Units (ICUs) often have a three- to four-month orientation period, where they learn the equipment, skills and patient management required in life-threatening illness. This training occurs after graduating from an accredited nursing program and passing the National Council Licensure Examination (NCLEX) for licensure.
Many states have proposed to graduate nursing students early to fill this critical staff shortage, and many schools of nursing have done so at some point during the pandemic. However, these novice nurses still need time to build their knowledge, confidence and efficiency in providing care and require the expertise and mentorship from experienced nurses and preceptors to do so. Experienced ICU nurses are responsible for caring for the sickest patients on the unit and may not be available to provide the orientation to these new nurses rushed into caring for critical patients amid a pandemic.
Contracted travel nurses are equipped to fill this staffing gap—however, with multiple epicenters nursing shortages simultaneously occurring nationally, the demand for experienced nurses are exceeding the supply. In addition, small rural hospitals may not have the financial resources to pay the steep wages that travel nurse agencies receive (often ranging from $4,000 to $10,000 per week), which leaves these hospitals at significant disadvantage to maintain an adequate work force. Even with hazard pay, hospitals across the nation are struggling to fill staffing holes.
Hospitals who do not contract travel nurses rely on their own staff to fill the gaps in the ICU. Nurses who work in general care areas, clinics or operative areas are being redeployed to care for higher acuity patients—often receiving just one to two days of orientation in units with different patient populations, technology and equipment than their usual work areas. This short orientation contributes to nursing burnout and poses risks to patient safety, as these nurses may not have the training or expertise yet to respond to acute changes in their patients.
Widening nurse-to-patient ratios also pose a significant risk to patient safety. Thorough assessment and monitoring of patients in the ICU requires that nurses care for fewer patients, where a nurse will care for only one or two patients (depending on the patients’ severity of illness). While only 14 states have laws or regulations that address nurse staffing in hospitals, California is the only state with laws that enforce nurse-to-patient ratios across all settings, with a ratio of one nurse to a maximum of two patients in the ICU.
Currently in California, these ratios are being exceeded, with ICU nurses caring for up to three patients after waivers were granted by Governor Gavin Newsom. This is occurring beyond the ICU; in general care areas, nurses previously cared for up to four patients and now are responsible for up to eight. Increased patient loads for nurses are occurring throughout the country. Since few states have regulations that mandate nurse-to-patient ratios, the waivers in California demonstrate the severity of the pandemic and nurses being spread thin.
Understaffing and COVID-19 affect quality of care and patient outcomes. This occurs outside of COVID-19 as well, as a newly published study indicated that each additional patient added to a nurse’s workload is associated with increased risk for dying in the hospital. With higher nursing workloads, nurses have less time per patient to provide care. This time deficit results in unintentional care omissions, such as reduced ability to closely monitor every patient, less patient education, incomplete documentation, late or missed medications or interventions, including those that maximize long-term recovery from critical illness.
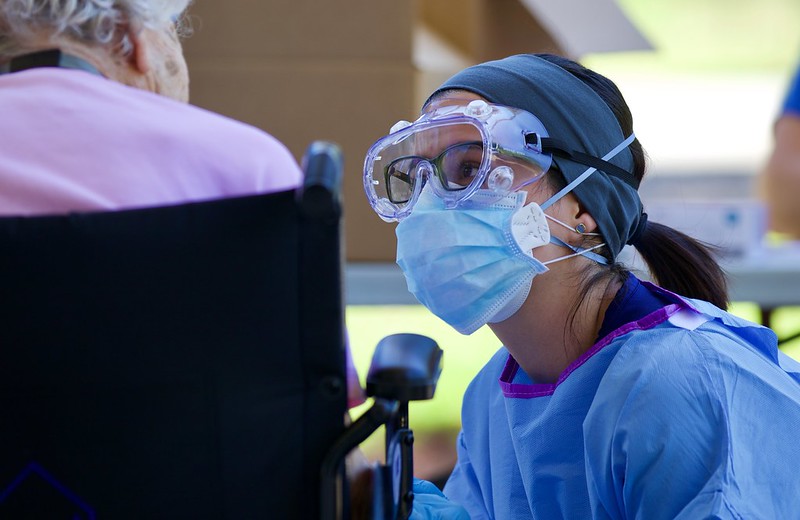
Patients with COVID-19 are often isolated from others due to visitor restrictions. Patients and families report that their only contact with each other is with or through nurses. Nurses facilitate contact between patients and families, often through videoconferencing. When nurses are spread thin, time cannot be spent facilitating communication for isolated patients. Isolation may contribute to worse depression, anxiety and confusion in health care settings, thereby worsening patient outcomes.
Nurses play a key role in contributing to optimal patient outcomes. High value-added nursing care is associated with shorter hospitalizations, lower health care costs, and better patient clinical condition. The value of nursing services is not routinely recognized, as the cost of nursing is embedded into the line item for room and board, rather than a separate line item that is visible to the patient, the public, and within the health care system. Because nursing is grouped with room and board, it continues to be easy to request “more beds,” and minimize the expertise required to care for patients in those beds. When expert nursing care is taken for granted and not actually available, patient care, safety and outcomes suffer.
Understaffing, high patient acuity and rapid training for non-critical care nurses contribute to burnout and a severe mental toll on the nursing work force. It is essential for both the media and administrators to recognize the contribution of nursing to the care of COVID-19 patients and differentiate between physical and human resources through appropriate language.
As recent events have demonstrated, the words used by the media and those in power matter. Without a nurse, a hospital bed is just a bed—and this should be clearly stated by the media and administrators. The nursing work force must be augmented through federal funding for surge staffing, comprehensive critical care training for redeployed non-critical care nurses, and evidence-based policies and pathways for augmenting the nursing work force amid disasters.
You may also like: