The challenges that women in medicine face were only exacerbated, not created, by the pandemic.

The COVID-19 pandemic has brought attention to the struggles of work-life balance, the reliance on women for many domestic activities, and the grueling hours and sacrifice health care workers make. If these issues were a Venn diagram, women in medicine would be at the center.
But the challenges that women in medicine face were only exacerbated, not created, by the pandemic.
The Majority of Medical Students Are Women—But This Is Not Reflected in Leadership Positions
In 2019, for the first time ever, the majority of medical students were women—an incredible accomplishment. Yet, looking at academic medicine, the percentage of women in leadership positions is far from the majority.
Furthermore, there seems to be an alarming correlation where the higher the academic rank, the smaller proportion of women there are. As a chart from the Association of American Medical Colleges (AAMC) shows, there is a 33 percent difference between the number of women who are full professors, one of the highest academic ranks, compared to women who are instructors, the lowest academic rank. In leadership positions in academic medicine, like deans of medical schools and department chairs, just 18 percent are women.
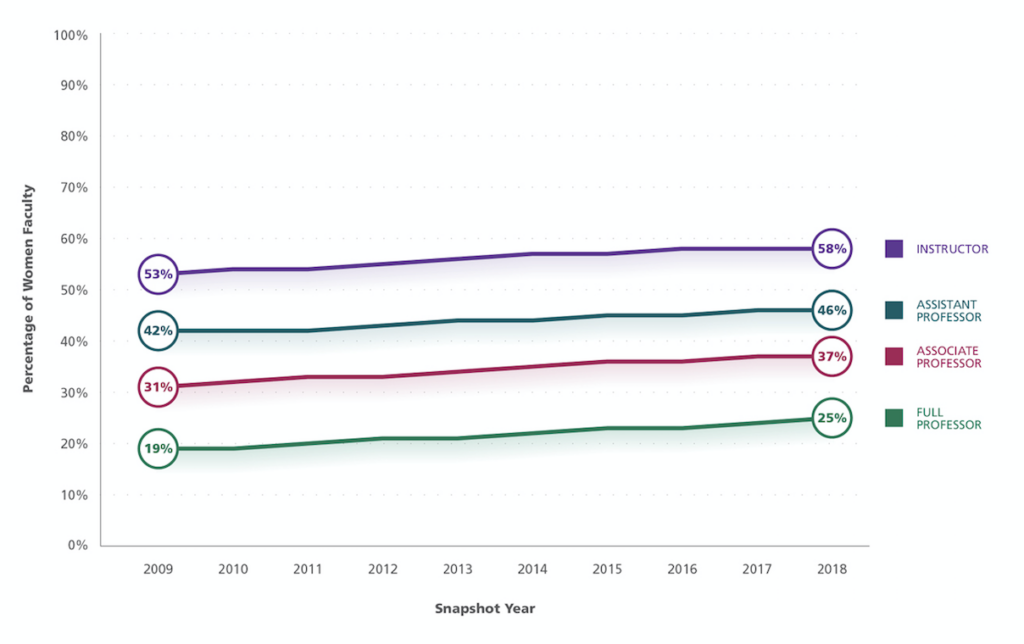
A lack of women in leadership positions means a lack of representation for creating policies that impact female physicians—like standardized maternity leave policies or extended time for breastfeeding during exams.
A medical student, Sophie Currier, had to file a claim against the National Board of Medical Examiners to get additional break time to pump during her medical licensing exam (ironically, the exam content actually includes topics on breastfeeding and its benefits). The case made its way up to the Massachusetts Supreme Court, where the judges agreed that not allowing lactating women extra time was unfair. Although the NBME have since changed their policies, it begs the question why it took so long—and a lawsuit.
Will the Pandemic Help or Hurt Women in Medicine?
The pandemic clearly has the potential to have long term effects on the careers of many women in medicine and further decrease the number of women in leadership positions. Dr. Kimberly Templeton, a professor at the University of Kansas Medical Center and past president of the American Medical Women’s Association, is worried the pandemic will cause women to “dramatically reduce their hours-—or leave medicine entirely.”
In fact, research has already shown how the pandemic is disproportionately affecting women in the field. To advance professionally in academic medicine and get those academic ranks, doctors are often expected to publish scientific research, which the COVID-19 pandemic has provided a wealth of opportunities for. When looking at the number of women who were the lead author in COVID-19 papers compared to previous years, the number was around 19 percent lower than expected. While the data was analyzing the early months of the pandemic (and there is some evidence that more women are publishing papers as the pandemic continues), it suggests that women initially may have had to forgo these opportunities.
Perhaps they were never even given the choice. In an article in JAMA, Dr. Linda Brubaker suggests that women are often passed on opportunities because they are assumed to have “a lot on their plate.” In regards to domestic duties, especially during the pandemic, female physicians typically do have more on their plate, with raising children and housework still falling more on women. Yet, ultimately, Dr. Brubaker argues, it should be the physician’s decision to decide what opportunities to pursue and what she can and cannot handle.
However, the one beneficial thing the pandemic has done is open up conversations about what it is like to be a woman in medicine. Just as the #MeToo movement revealed longstanding problems of sexual harassment, the pandemic has revealed the longstanding problems of women getting penalized at work for raising a family at home (or even expectations that they will one day raise a family).
Thus, Dr. Brubaker sees the pandemic as a “potential catalyst” to ensure medicine has a healthier work-life balance—not only for female physicians, but for all physicians.
But to accomplish this, we must ensure the pandemic does not push women in medicine, who bear the brunt of work-life conflicts, out of leadership positions and out of the field. In fact, we need their voices and perspectives now more than ever before.
Up next:





