In male-dominated fields, women continue to be undervalued in the workplace.

Update May 10 at 7:01 a.m. PT: Goldman Sachs agreed to pay $215 million to settle a class-action lawsuit that alleges the bank systematically underpays and undervalues women. The settlement will pay out roughly 2,800 women employees in various divisions at Goldman, where men continue to outnumber women and dominate senior roles.
“I have been proud to support this case without hesitation over the last nearly 13 years and believe this settlement will help the women I had in mind when I filed the case,” said Shanna Orlich, one of the women who first filed the legal complaint.
Goldman Sachs will be headed to court next month to battle a class of current and former female employees who assert they received lower pay and weaker performance reviews as a result of pervasive gender discrimination, stifling career growth.
The Goldman case stretches back to actions the company took in 2002 and 2004, and it’s tempting to believe that whatever gender bias sins the investment bank allegedly committed over a decade ago would never happen now.
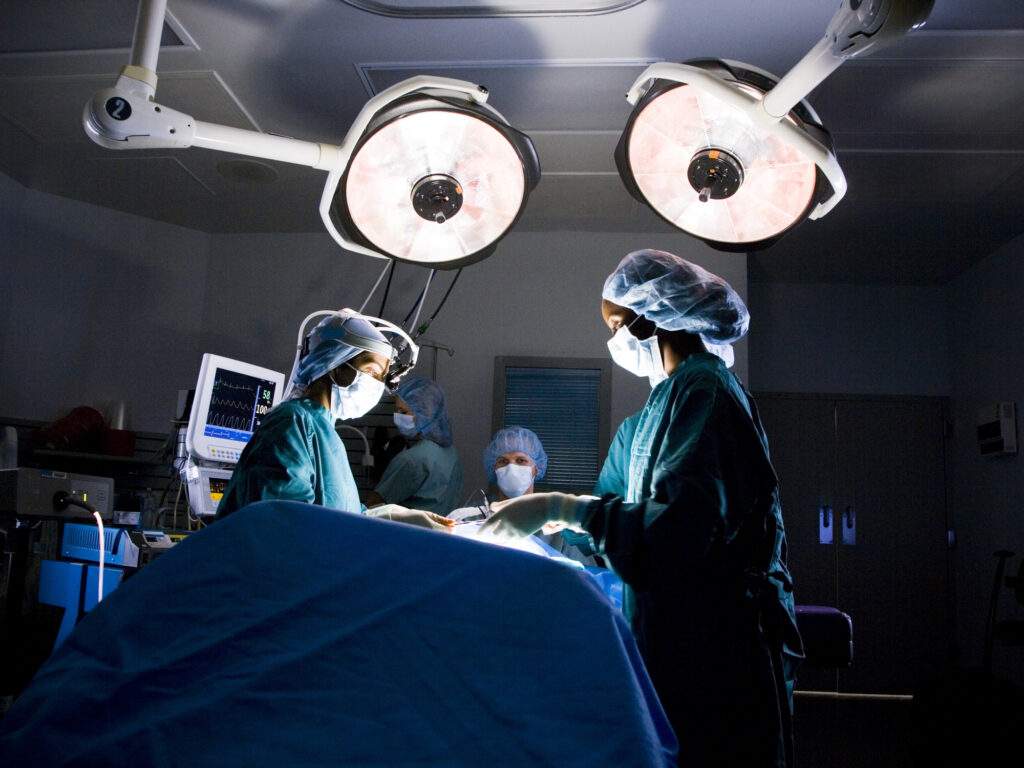
But in another male-dominated field—surgery—recent data show that women continue to be undervalued in the workplace. Like Goldman executives, faculty at the University of Washington rated their senior female residents significantly worse than their men. According to faculty, senior male residents outshone the women in nearly every category: knowledge of surgical diseases, operative knowledge, professionalism, health and well-being, and administrative tasks. A solitary woman scored high in one category: patient and family-centered communication. The sample size was small, but a larger, multi-center study in emergency medicine also found that faculty—both male and female—favored male residents. They felt the women they were rating lacked confidence in procedural skills.
A male standard is the default in fields built by men for men, like surgery.
It looks pretty bad for women. But if you ignore those faculty opinions and look at studies of actual patient outcomes, you’d find something entirely different. Patients with diabetes, heart attacks and other causes for hospital admission fare better with female physicians, not worse. And surgical patients in the U.S. and Canada, particularly women, have better outcomes with female surgeons.
Why the difference? We can only guess, but perhaps their softer, more ‘feminine’ qualities—the very qualities that might be contributing to those lower faculty evaluations—gave women an advantage in the practice of medicine. After all, studies have shown that women physicians are more likely to explore patients’ social circumstances, collaborate with colleagues and follow guidelines.
If institutions use opinion-based evaluations to determine promotions and competence, then they should recognize the biases baked into those opinions. Sadly, many diversity programs that aim to shed light on those biases often fail and sometimes even backfire because they work at the cognitive level—raising awareness—without the emotional engagement that drives the urge to change.
A male standard is the default in fields built by men for men, like surgery. Years ago, as a plastic surgery resident, I protested the knowledge-category score that one of my professors had given me. Only after I told him I had received a 99 percent on a national examination did he relent. I realized my nickname, ‘Giggles,’ wasn’t working in my favor. Later, communication experts at women surgeons’ symposiums warned us against making suggestions the way women often did—the way I did: “Maybe we could consider…” or “Perhaps we could try…”
It turns out I was setting myself up to be ignored or uncredited. Why wasn’t anyone teaching the men to talk like women?
Unconscious bias disproportionately drives female students away from surgery. With its lengthy training system (five or more years longer than primary care specialties), surgical specialties retain a military-like hierarchy with a pro-male gender bias that increases career engagement among male residents, possibly contributing to their higher academic performance. A qualitative systematic review of gender bias in surgery found that female surgeons feel more closely scrutinized for mistakes, and to fit in, some compromise their female identity, even engaging in lewd remarks with their male colleagues. Maternity leave is stigmatized, even by female superiors, and female surgeons observe gender disparities in pay and advancement, despite being equally qualified.
Among women who do train in surgery, one in four quit—significantly more than men—and those who finish are significantly less likely than men to become board certified. And their substantial attrition up the academic ladder narrows the female representation from 29 percent at the bottom rung (assistant professor) to 6.3 percent at the top (chair).
At Goldman, the share of women employees reached 42.2 percent in 2021, yet its senior management remains static around 23 percent. Are so many women really not qualified for promotion?
We need unbiased information—data, not opinions—to find out. Too many institutions evaluate people like the scouts described in Michael Lewis’s Moneyball: The Art of Winning an Unfair Game, the ones who fought with their stats-obsessed general manager, Billy Beane. They knew the way a baseball player should look—”like an athlete”—just the way the surgery and emergency medicine faculty know how surgeons and E.R. docs should look, talk and act. And yet, the data shows that the underdogs—the soft-bodied players and the under-scoring women—perform better than the rest. If we give them a chance, everyone wins.
On June 5, Goldman Sachs may wish they’d had a Billy Beane.
Up next:
U.S. democracy is at a dangerous inflection point—from the demise of abortion rights, to a lack of pay equity and parental leave, to skyrocketing maternal mortality, and attacks on trans health. Left unchecked, these crises will lead to wider gaps in political participation and representation. For 50 years, Ms. has been forging feminist journalism—reporting, rebelling and truth-telling from the front-lines, championing the Equal Rights Amendment, and centering the stories of those most impacted. With all that’s at stake for equality, we are redoubling our commitment for the next 50 years. In turn, we need your help, Support Ms. today with a donation—any amount that is meaningful to you. For as little as $5 each month, you’ll receive the print magazine along with our e-newsletters, action alerts, and invitations to Ms. Studios events and podcasts. We are grateful for your loyalty and ferocity.





