Update on March 30 at 7:06 a.m. PT: Listen to the 2-minute broadcast version of this story, read by Lily Böhlke for Illinois News Connection, reporting for the Ms. magazine-Public News Service Collaboration.

As we await the fate of Roe v. Wade, Ms.’s “Online Abortion Provider” series will spotlight the wide range of new telemedicine abortion providers springing up across the country in response to the recent removal of longstanding FDA restrictions on the abortion pill mifepristone.
Melissa Grant is the chief operations officer of the abortion provider carafem, which opened their first abortion clinic in the Washington, D.C., metro area in 2015 and began offering telemedicine abortion in Georgia in 2019 through Gynuity Health Project’s TelAbortion study. Early in the pandemic, they expanded their TelAbortion services to Illinois and Maryland. In July of 2020, when a Maryland federal court lifted an FDA in-person distribution requirement for the abortion pill mifepristone, carafem expanded the service to still more states.
carafem now offers telemedicine abortion in 11 states—Connecticut, Georgia, Iowa, Illinois, Massachusetts, Maryland, Nevada, New Jersey, Rhode Island, Virginia and Vermont—plus the District of Columbia.
Ms. spoke to Melissa about how and why carafem began offering telehealth abortion services.
Carrie Baker: Could you tell me about your background and practice?
Melissa Grant: I’m an administrator at carafem, which I founded eight years ago. We are a network of family planning and reproductive healthcare clinics that started in Chevy Chase, Maryland, a couple blocks from Washington, D.C.
The idea behind carafem was to see what we can offer that might be different than the way abortion care was traditionally provided in the U.S. in an effort to make abortion more accessible. Where I had worked previously, it was not uncommon for large groups of people to come in for care and have it take maybe four or five hours to receive it. We focused on client-centered where the client calls the shots. In one-on-one conversations, we review how each person wants to receive care, let them lead the conversation, and don’t interrupt them. And that has been successful—both in person and online.
Baker: How many telemedicine abortion patients have you seen since the FDA restriction was lifted in July of 2020?
Grant: We’ve provided high-quality, safe and effective telehealth abortion care to several thousand clients.
Baker: How do your patients find you?
Grant: We developed a really strong and unapologetic presence out in the community about the fact that we’re an abortion care provider. What we’ve found is that one of the first places people go when seeking abortion care is Google, so we focus ad budgets and create content that meets clients where they are. We also use social media and outdoor ads at certain times.
We are crystal clear about what we do. Hence the tagline, “Abortion. Yeah, we do that.” Many of our clients publish reviews on Google or Yelp, which we share far and wide to let our clients speak to our level of care.
Baker: So once a patient gets to your website, tell me about the process.
Grant: They can either make an appointment through our website (carafem.org) or they can call us. We are open six days a week from about 8 o’clock in the morning till 8 o’clock at night. We have English and Spanish speaking agents, as well as translation services for multiple languages to try and be as welcoming and inclusive as possible.
Baker: Once somebody makes an appointment, what happens next?
Grant: If they live in a state where there’s not a state-mandated waiting period, they could potentially make an appointment on the same day and meet with a carafem clinician online that same day. In some states, for instance Georgia, there’s a 24-hour waiting period that’s required. With a telemedicine appointment, you can schedule it on the phone, or you can schedule it as a video call.
Then, we send some forms to fill out ahead of time and some information about the process. We collect their health history. To get ready for the informed consent process, we send information about risks, alternatives and benefits. That all can be done online through secure email if they have the ability to use email. We have an option where you can click a link from your smartphone to access the forms and educational information. If they don’t have access to email, they can call us and we will review the information over the phone.
At the time of your appointment, you click a unique link and you’re in a virtual waiting room. There’s some information in there to read through while you’re waiting, though most people don’t wait more than a couple minutes. It’s a fully private room—no one else will be in the waiting room with you. Then a care coordinator signs in and joins your visit. It’s a secure video conference platform that’s made specifically for telehealth visits.
During that time, we review your health history, talk about how the medicines work, when you will take them, how to know if they worked or not, how to know when you need to contact us, and what our follow up process will be like. We talk about birth control. The whole thing takes maybe 15-20 minutes, if that.
Then we bring a physician onto the call to review the informed consent, make sure the client understands how to use the medications, and give the client the opportunity to ask questions. That’s usually fairly simple. At that point, the physician approves the prescription that is then electronically sent to an online pharmacy.
Baker: How long does it take to get the abortion pills?
Grant: Most clients receive their medication within a day to three days. If they want it sooner, we can expedite. They will receive a tracking number, generally within a few hours, and they can track the medication on its way.
Baker: On your website, you say you send the pills in discreet packaging. What does that mean?
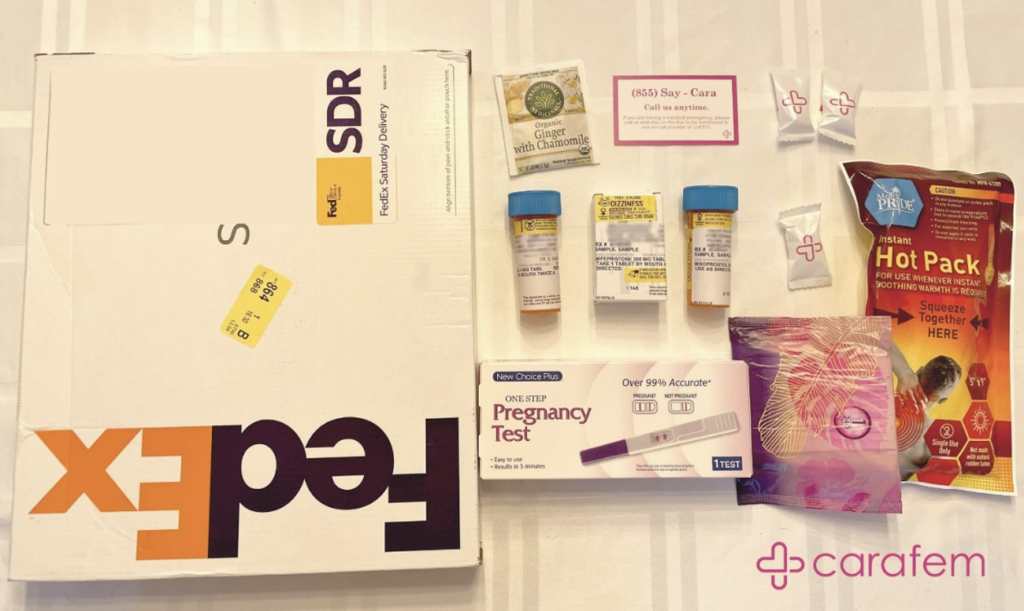
Grant: Oftentimes one of the concerns that our clients have is, “When this is delivered to my mailbox, what will it look like?” We use a plain shipping box. It does not have our address on it. It has a P.O. box return address or the address of the pharmacy in the corner, and it doesn’t say what it is. And if they live in a circumstance where they can’t get mail, we can arrange to have it sent to a shipping service in their community like UPS or FedEx or a drop box, and they can go pick it up.
We send the mifeprex package, and we also send along a few mints because the medicine tastes bad, some herbal tea—sometimes tea settles tummies, a heating pad, a pad to get you started, some anti-nausea medications, some ibuprofen, a pregnancy test and basic birth control if you want it. And some educational materials. We’ve heard from many clients that they appreciate the little extras in our package.
Baker: What kind of follow-up care do you provide?
Grant: We conctact every single one of our clients generally within two to three days after taking the medication. We set that up beforehand. For some of our clients, they actually prefer to use a text-based system so they can text us if they want.
We want to know a few things. Did you take the medication successfully? Did you see cramping and bleeding? Did things seem within the normal expectations that we discussed for cramping and bleeding? We want to make sure it’s not too much, and not too little bleedng. Are you starting to see a decrease in pregnancy symptoms? And do you feel like you had a complete abortion?
If all those answers are yes, we see if there are any other issues. If they wanted a birth control method, we make sure they’ve taken that or are about to take it or know how to take it. We also include a pregnancy test in the package they receive and ask that about four weeks out if they took the test and to send us the result.
Baker: Do they do that by text usually?
Grant: They can do it by text, by phone or by portal. If we don’t hear from you, we’ll give you a call and ask.
Baker: What percentage of folks follow up and how?
Grant: The majority of clients follow up because we contact them proactively. That first phone call is when we identify most problems, like needing more medication or needing to come into one of our clinics. It’s very rarely urgent. Less than 0.4 percent of our clients have a problem where they would require treatment of any kind. Less than 2 percent have any kind of concern about an ongoing pregnancy.
Baker: Do you have appointments at night and weekends?
Grant: We do. We have physicians and nurse practitioners that are licensed across the U.S. So for different time zones, we have different people that take shifts that can actually help to do follow up for any of the communities that we’re in.
Baker: What do you charge for telemedicine abortion services?
Grant: Between $250 and $375 out of pocket, depending on medication. We offer financial assistance to those who qualify. In some of our communities, we take Medicaid, such as Illinois. We also take private insurance. We also work with abortion funds, organizations that provide financial assistance for abortion care.
If you have a concern about paying, we ask that you give us a call. Our staff are really, really good about working with people to find options.
Baker: If someone has trouble paying, do you work with them?
Grant: If you have a concern about paying, we ask that you give us a call. Our staff are really, really good about working with people to find options. We have a relationship with many of the abortion funding organizations. If we’ve collected the information that they need, we can contact a fund and then get back to a client saying we’ve secured funding for you and this is how much we ask that you to bring.
Baker: Do you offer advance provision abortion pills?
Grant: We don’t now but we are undergoing a thorough analysis on a state by state basis to understand legal and medical implications.
Baker: Do you offer missed period pills?
Grant: Yes, we do. We actually were doing a Gynuity study in D.C. last year on missed period pills that temporarily paused during the pandemic. We have had clients who tell us, “I can tell you when my last period was. I’ve not had a positive pregnancy test. I prefer not to.” We let them know clearly, if you do this and you’re pregnant, it’s an abortion, and if you do this and you’re not pregnant, you’re taking medication that you probably don’t need. We tell them the risks, however small they may be, and ask, “Are you comfortable with that?” The key is making sure that that client is fully aware of what this medication will do one way or the other.
Baker: Can you tell me about who your telemedicine abortion patients are?
Grant: We’re seeing more people from rural communities, micropolitan areas and small towns. During the worst of the pandemic, we saw many more low-income clients. Now, as other healthcare professionals are finding out, we’re seeing telehealth numbers shift a little bit as people are going back in for healthcare, face to face.
Baker: Why do your patients say they are using telemedicine abortion?
Grant: The most common answer that we hear is it’s easier. They don’t have to travel. Childcare is an issue. During the pandemic, it was limiting their exposure to other people. Lately, I’ve been hearing it’s more discreet and more private to be able to do it from home. We have people that do the meeting from their living room, we have people that do it in their office, we have people who’ve done it at a public library on a computer. People can do it on their smartphone in the bathroom. And then cost, it’s less money. Generally, the average cost for an in-person visit is close to $500.
We hear is it’s easier. They don’t have to travel. Childcare is an issue. During the pandemic, it was limiting their exposure to other people. Lately, I’ve been hearing it’s more discreet and more private to be able to do it from home.
Baker: Have any of them said that they are having a hard time getting prompt appointments at traditional providers?
Grant: Yes, we’ve heard that more recently, especially since S.B. 8 in Texas.
Baker: Are people driving from Texas to the states you serve and doing telemedicine on the borders?
Grant: Not Texas yet, but I’ve seen it from other states like Louisiana where people have driven into Georgia because all providers in Louisiana are full. I have seen people from Oklahoma who’ve gone to Illinois.
Baker: Do any of your patients mention not wanting to cross picketers and protesters?
Grant: Some do. carafem offices are located within multi-use medical facilities with several other medical offices (like dentists, family practice providers, etc.) so we are not as challenged by protesters as we would be in a stand-alone building. We certainly hear it from people who don’t have a private clinic in their area and it’s a concern. And it’s certainly greater in the South and the Midwest than the rest of the country.
Baker: What do your patients say about their experiences with telemedicine abortion? Are they having good experiences?
Grant: Yes. We ask them, “Would you recommend carafem to a friend or family member?” and “Do you feel treated with kindness and respect?” Overall, 95 to 99 percent of our clients agree or strongly agree on those two questions. It’s incredibly moving to hear when we’re able to meet a need or exceed expectations. It’s amazing, especially when someone, because of stigma, assumes that this experience is going to be terrible or assumes that they may be judged.
And that’s honestly one of the harder things about the telemedicine space. We have had some clients who’ve said straight out that the reason why they chose telemedicine is because they were afraid they would be judged by a healthcare provider going in person. And that was really, really tough for us to hear. We do everything that we can do to try to prevent that. But medicine in the United States is hard. And this particular type of medicine is harder than many others. There is judgment and there is a lot of stigma associated with even talking about birth control, much less abortion care. It shouldn’t be that way.
Baker: What are your motivations for offering telemedicine abortion? Why do you do this?
Grant: The main reason is to try to make sure that people who need this care can continue to receive it. People should be able to get abortions in the way that makes the most sense to them. And sometimes in their communities, they can’t. We do this because states around the country have started to shut down the opportunity to receive abortion care. The laws that have been passed in this country in the last year—more than 100—have restricted abortion care in some areas to the point where it’s almost completely inaccessible.
Baker: How does it feel to be able to offer this service to people?
Grant: On one hand it’s freeing because people sometimes will start off and say: Are you a real abortion provider? I can say, “Yeah we do that,” which is wonderful.
But at the same time disappointing, because we should not have delegitimized this needed and legal form of healthcare to the point where we can’t get it another way. People should be able to receive care in a way that they need it and want it. Telemedicine abortion is a direct result of trying to find a workaround. It’s part of that giant chess game that abortion providers have to play in order to continue to provide care. Yes, if it’s better, that’s wonderful. It’s not always and it shouldn’t be the only option. There are 19 states that ban telemedicine outright. That’s not right. People are now deciding if they’re going to self-manage an abortion with drugs that are imported from other countries because they can’t even get telehealth abortion care in some states. I’m not saying it’s not safe. They may be having good experiences, but oftentimes it’s very slow.
We have taken a tremendous step backwards in this country in the past 10 years, even more so in the last year. I continue to be surprised, deeply saddened and concerned about what’s going to happen to the people who depend on us for care in states that are severely limiting access.
Baker: What difference did the FDA lifting the in-person requirement for the abortion pill make to you?
Grant: The biggest thing is that it assures us that we’ll continue to be able to provide abortion pills through the mail even after the pandemic is over. This will help increase access to abortion care to more people.
Baker: Any final thoughts?
Grant: Medication abortion has been legal for over 20 years in the United States. Abortion has been legal for nearly 50 years in the United States. We have taken a tremendous step backwards in this country in the past 10 years, even more so in the last year. I continue to be surprised, deeply saddened and concerned about what’s going to happen to the people who depend on us for care in states that are severely limiting access.
Access to healthcare should not be determined by how much money you make, or what side of a state border you live on, or what your religious beliefs are or the color of your skin. We should all be able to get healthcare that is safe and dignified, and respects the individual differences that we have. You can’t get that right now with abortion care in the United States. And some people have settled for the next best thing for a long time. People think, this law didn’t mean anything. That law didn’t really mean anything. We can still generally get care. But we’re at a tipping point now. It’s time for folks in this country to wake up. I believe the majority of people want abortion care to remain legal, so their friends, family, and community members are able to receive care that’s safe, nonjudgmental and respectful of them as a human being.
Sign and share Ms.’s relaunched “We Have Had Abortions” petition—whether you yourself have had an abortion, or simply stand in solidarity with those who have—to let the Supreme Court, Congress and the White House know: We will not give up the right to safe, legal, accessible abortion.
Explore the full collection of online abortion providers profiles:
- Dr. April Lockley Answers Your Questions About Abortion Pills: ‘To Protect Each Other As Much As We Can’, Ms., March 16, 2022
- Online Abortion Provider Razel Remen: ‘Telemedicine Abortion Is Safe and Reliable’ Ms., March 2, 2022
- Telemedicine Abortion Provider Rebecca Gomperts Gets Abortion Pills Into the Hands of Those Who Need Them: ‘It’s a Privilege’ Ms., Feb. 23, 2022
- Telemedicine Abortion Provider Alison Case: “Helping People in Texas Access Abortion Care” Ms., Feb. 15, 2022
- Telemedicine Abortion Provider Melissa Grant: “Abortion? Yeah, We Do That.” Ms., Feb. 2, 2022.
- Online Abortion Provider Christie Pitney of Forward Midwifery: “Fast, Convenient Care,” Ms., Jan. 28, 2022.
- Online Abortion Provider Julie Amaon of Just the Pill Is “Making Abortion as Easy as Possible for People,” Ms., Jan 26, 2022.
- Online Abortion Provider and “Activist Physician” Michele Gomez Is Expanding Early Abortion Options Into Primary Care, Ms., Jan. 19, 2022.
- Online Abortion Providers Cindy Adam and Lauren Dubey of Choix: “We’re Really Excited About the Future of Abortion Care,” Ms., Jan. 14, 2022.
- Telemedicine Abortion Provider Dr. Deborah Oyer Supports Patient Autonomy and Control: “No Different Than When They’re in Clinic,” Ms., Jan 12, 2022.
- Online Abortion Provider Robin Tucker: “I’m Trying To Remove Barriers. … It Feels Great To Be Able To Help People This Way,” Ms., Jan. 4, 2022.
- Abortion on Demand Offers Telemedicine Abortion in 20+ States and Counting: “I Didn’t Know I Could Do This!” Ms., June 7, 2021.
Up next:





