The end of Roe, combined with existing anti-poor fertility policies, means that women—especially poor women of color—will have even less of a say in the time and circumstances in which they decide to have a family.
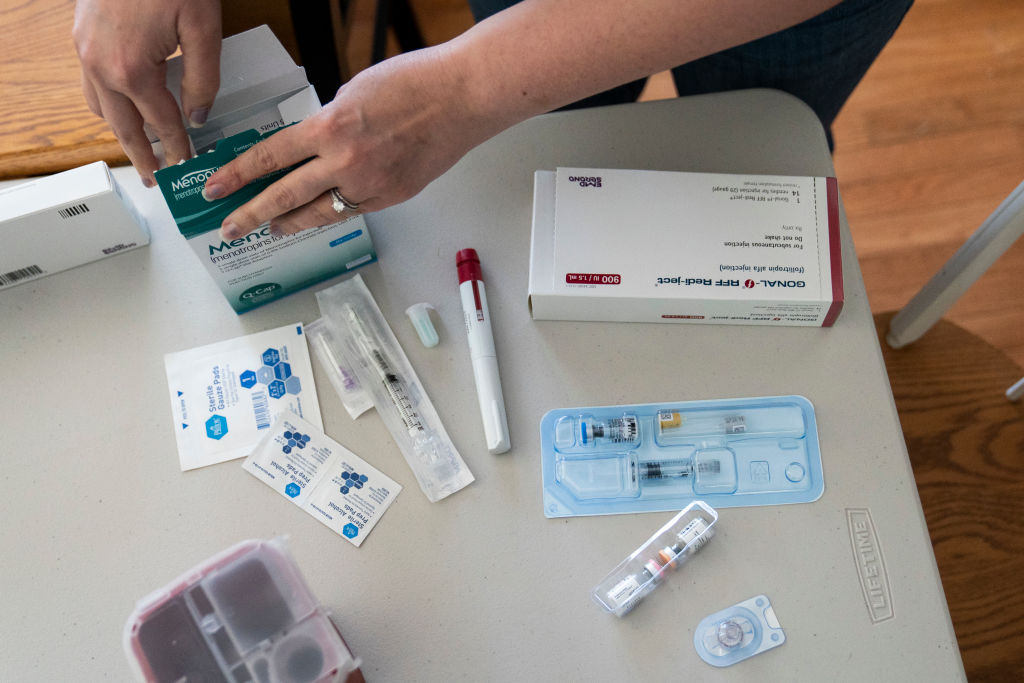
It’s no coincidence that the world’s first IVF baby was born just five years after the 1973 Roe v. Wade decision. IVF, or in vitro fertilization, is often mistakenly thought to be irrelevant to abortion debates. After all, people spend tens of thousands of dollars on reproductive technologies like IVF to help them become pregnant, while the conversation surrounding abortion largely concerns unexpected and often unwanted pregnancies.
But, upon a closer look, Roe not only empowered millions of women with bodily autonomy by constitutionally protecting their right to terminate a pregnancy—the decision also enabled the rapid growth of new technologies beyond IVF to assist human reproduction.
With Roe reversed, several states are poised to ban abortions; trigger laws in at least 13 U.S. states will immediately prohibit abortion without exceptions. Under many of these state laws, ‘life’ will be defined as the moment an egg is fertilized. These laws threaten those undergoing (and those performing) procedures, such as IVF or third-party gamete donation, by limiting or prohibiting the freezing or discarding of embryos—a process fundamental to successful fertility treatments. Researchers will likely face insufficient access to embryos to improve available treatments. Overturning Roe infringes upon the ability to preserve or willingly discard embryos. These practices, which are central to safe advancements in fertility medicine, could all but vanish in some places.
In fact, the overturning of Roe will dramatically limit a crucial option for many people looking to build families. Technologies such as IVF help thousands of people have children every year in the United States. Between 2018 and 2019 alone, there was an almost 4 percent increase in babies born using IVF in the U.S., signaling how integral these fertility options are to families.
Because fertility processes can be arduous, risky and costly, doctors typically try to create multiple embryos from a patient’s single cycle of treatment. Fertility scientists must also be able to study embryos, which requires being able to store, freeze and discard embryos in order to make assisted reproduction safer and more effective. Without Roe, each of these processes enabling fertility care are in jeopardy in jurisdictions that do not support abortion rights.
Overturning Roe infringes upon the ability to preserve or willingly discard embryos. These practices, which are central to safe advancements in fertility medicine, could all but vanish in some places.
Abortion and assisted reproductive technologies share another commonality: Women’s access has always been patterned along racial and class lines. And the end of Roe could only further entrench this. Individuals from marginalized groups have historically faced multiple barriers to fertility treatment including cost, lack of insurance coverage and discrimination by providers.
In fact, there are no federal requirements for state Medicaid programs to cover fertility testing or treatments, meaning that most low-income women on Medicaid often have mandatory contraceptive coverage, but no coverage for fertility treatments. The result is that while women of color face higher infertility rates, they utilize ARTs at significantly lower rates than white women, who are twice as likely as Latina women and four times as likely as black women to use ARTs.
In other words, the end of Roe, combined with existing anti-poor fertility policies, means that poor women of color will have even less opportunity to determine the time and circumstance in which they decide to have a family. Reproductive justice movements have been working tirelessly to avoid this very scenario, which is why the decision to overturn Roe is so incredibly unjust.
Dismantling reproductive autonomy will inevitably create challenges for America’s disabled children and their families. Currently, preimplantation genetic testing (PGT)—a relatively common fertility practice—allows hopeful parents to test their embryos for particular genetic conditions. This kind of genetic testing can increase the likelihood of a successful pregnancy, while averting the expense and heartache of a miscarriage or multiple failed attempts at conception.
If embryos represent ‘life,’ however, these kinds of reproductive choices could disappear altogether in some states. Parents may have to implant embryos that are unviable, leading to pregnancies bound to fail, or find themselves with children that have genetic conditions they are unable to care for. The loss of Roe could thus exacerbate both the financial and emotional toll of fertility care and leave families with disabled children unsupported.
While those well-off may be able to afford alternatives, many fertility patients could be faced with laws prohibiting embryo selection or abortion based on genetic conditions. The result? We may find genetic mutations concentrated in poorer communities of color, where alarming numbers of children already cope with environmentally induced disabilities. Given the severe lack of social supports in the U.S., those who are under-resourced would struggle most to afford adequate care for their disabled children. This could worsen financial, educational and health disparities for children with genetic conditions, not to mention entrenching the stigma surrounding disability.
Overturning Roe will impact everyone. However, the permeating loss of reproductive autonomy will have a profound effect on making fertility medicine and family-planning more inaccessible, unequal and unfeasible for women of color, low-income families and families with disabilities.
What’s especially disturbing is that these restrictions emerge at a moment where fertility technology is becoming ever more precise. For those who can purchase private healthcare, accommodation and travel to states that protect bodily autonomy, the options for managing one’s fertility and reproductive outcomes remain rather plentiful. And with new (albeit controversial) technologies like CRISPR-Cas9 and polygenic embryo screening at the front door of fertility care, the gap between the haves and the have-nots only widens. While an existing privileged class can continue to enjoy fertility advancements, those left behind face the brunt of social neglect.
Without the protections of Roe, we stand to see gross inequalities in fertility care and reproductive decision-making. Paradoxically, these devastating impacts will hurt those who want to have children, exacerbating unequal access to fertility resources and creating societal inequities in a manner not seen in decades.
Sign and share Ms.’s relaunched “We Have Had Abortions” petition—whether you yourself have had an abortion, or simply stand in solidarity with those who have—to let the Supreme Court, Congress and the White House know: We will not give up the right to safe, legal, accessible abortion.
Up next:





