
Since the cataclysmic Supreme Court decision to overturn Roe v. Wade, doctors and clinicians are reporting an increase in demand for different forms of contraception, including emergency contraception like Plan B and Ella, and longer-lasting forms of birth control like IUDs and birth control implants. But legislation defining life as beginning at fertilization, proposed at the national level and in at least eight statehouses around the U.S, puts contraception access at risk.
Especially in this time of crisis, Dr. Sophia Yen says it’s essential we take charge of our own reproductive health. Yen is the CEO and co-founder of Pandia Health, the only doctor-led and women-founded and -led birth control delivery company. She is a board-certified physician with a focus in adolescent medicine, and serves as a clinical associate professor at Stanford Medical School in the Department of Pediatrics. Yen co-founded Pandia Health because she believes no one should suffer from “pill anxiety”—the fear of running out of birth control and the stress of having to obtain birth control each month. Her latest health campaign is to educate the public about #PeriodsOptional.
In a Ms. webinar on Tuesday, “Everything You Ever Wanted to Know About Birth Control,” Yen broke down the best forms of birth control and emergency contraception, why you should consider skipping your period, how to get abortion pills (even if you live in a state with a ban), and more.
Below, find a recording of the event, plus a transcript, lightly edited for clarity.
Dr. Sophia Yen: It’s so great to see such a huge audience turn out for this talk.
First of all, if you all don’t know about it, please know about PlanCPills.org. I use my social media as a platform for public service announcements, so feel free to call this a Pandia public service announcement or just a public service announcement via Ms. Magazine, but everybody should check out PlanCPills.org. It’s a nonprofit and it has anything and everything you could possibly want to know about medication abortion, which can be done technically up to 10–12 weeks after your last menstrual period. If you go to the website, you type in your state, it will tell you what telemedicine providers are legally allowed to serve you in your state.
My 5 tips about #abortion now that #RoeVWade is over.
— Sophia Yen MD (@teenmd) June 24, 2022
1. Get your birth control under control. Get it delivered by @PandiaHealth or get an IUD or implant or vasectomy
2. know about https://t.co/Pin6qMHbaI @Plancpills
3. check https://t.co/hzw7W2JzeM
more to follow…
They work with Aid Access. They are by Dr. Rebecca Gomperts of the Netherlands, and she will never come to the U.S. so that she can’t get sued or extradited. She writes the prescriptions in the Netherlands, the medicines come from India and that’s why you see it’s a 14 to 21 day delivery period, but she can service all states, and it’s only $110 for the doctor support and the medication.
One radical thing that my friend who founded PlanCPills, Dr. Francine Coeytaux says is that you can consider getting the pills in advance of need. You can skip checking a pregnancy test—just if you miss a period, take these medications and it just brings your period, so the issue of abortion never comes into play. It’s just making your period regular, for those states that are more restrictive or that have anti-abortion laws out there.
They can also connect you with free medical hotlines you can call if you have any questions about medication abortion. There’s also a legal hotline that’s free, that’s staffed by If/When/How, which was formerly Law Students for Choice.
And then number two, make sure you know about the website “After Roe Fell: Abortion Laws by State” from the Center for Reproductive Rights, and it pulls up this map. Green is expanded access, yellow is protected, and then orange and red and really dark red are not good, and as you can see here, 26-plus states are really not good. Then you can click on the specific state for up-to-date laws, such as waiting periods or six-week ban or 10-week ban or 12-week ban, so this is just a great resource if you’re doing state-to-state advocacy.
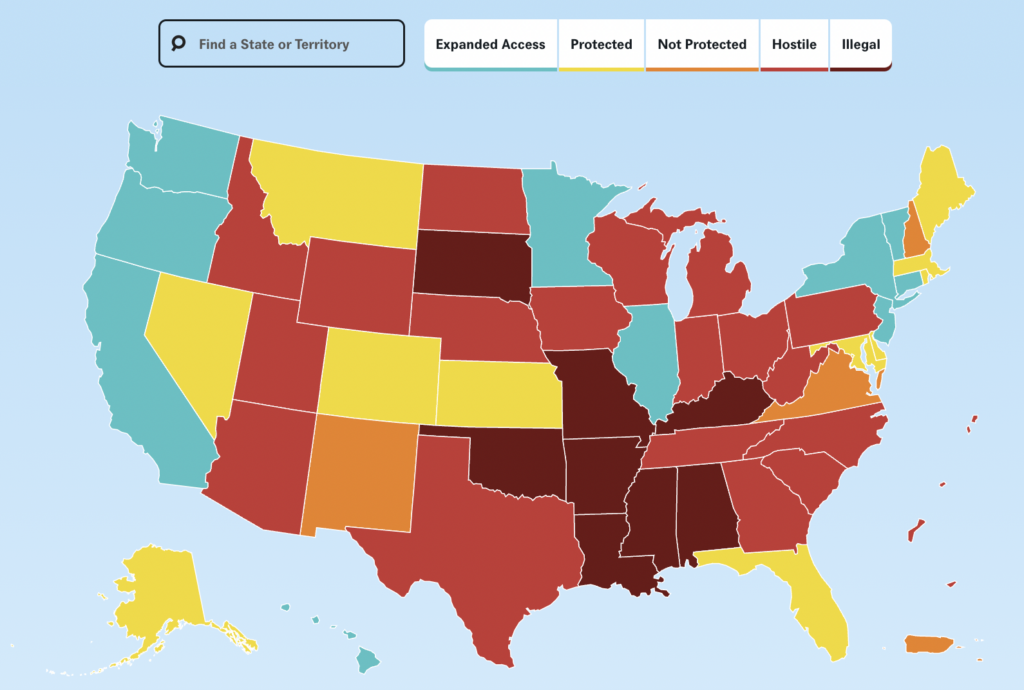
And then there’s the National Network of Abortion Funds and the National Abortion Federation. There are lots of crisis pregnancy centers out there, and if you do a Google for abortion clinic, 20-25 percent of what comes up are these crisis pregnancy centers. They don’t really have any medical staff, they tell women lies about abortion—if you get an abortion, you’ll end up sterile or you’ll become a drug addict, or all sorts of crazy things.
But these are two trusted websites. On the National Network of Abortion Funds, you go there and you can ask for money by state, and if you have money, you can donate money by state or you can donate it in general. The National Abortion Federation is a group of abortion providers that are safe.
Number four, delete your period apps if you are in any of those states that are not friendly. People are like, “But they say they’ll protect my data,” or whatever. Uh-uh. I went to MIT and I have friends that do forensic computer stuff, and as long as if it was ever on your phone, ever on your computer, or if your phone ever uploaded to the Internet, which pretty much all our phones do, then they can find that information. So, unless you only keep it on your laptop, desktop and then you crush that sucker and then you throw it into the ocean, which would not be good for the ocean, then if at any time you would consider doing a termination, then you should delete your period apps. If termination is not in your future, then don’t worry about it, but if it would ever be a concern, perhaps sexual assault, God forbid, then that is something you really need to take into consideration.
Optimize your birth control. The implants beats vasectomy, which totally blows my mind. That’s something you put in your arm, lasts for three years, can beat the snip-snip. And then the IUD with hormone beats tubal ligation. I think it’s crazy enough that your body could get pregnant on tubal ligation, because it’s not just snip-snip, burn, it’s snip-snip, take out an inch, tie, and burn, and you still get pregnant on that, and the IUD with hormone beats that.
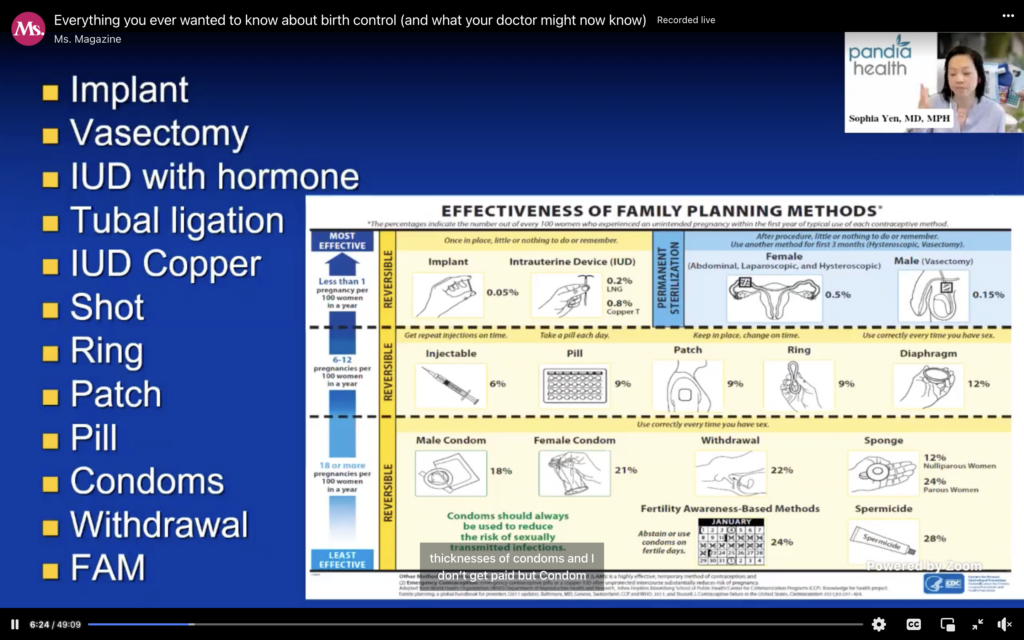
And then next comes up the copper IUD. Make sure you know if you’re on the copper IUD that the two major side effects, and there were a lot of copper IUD users on this call, are more blood, more cramps, and so if you’re the kind of person who feels every single cramp, maybe not the copper IUD. If you’re the person who bleeds like stink, maybe not the copper IUD. If you’re the kind of person who’s like, “Oh, is that blood? Is that my period?” Yes. You. You, the copper IUD. So, the copper IUD is amazing in that it lasts out for 10 years. The IUD with hormone can last from five to seven years.
Then comes the shot, the ring, the patch, the pill, and the only reason the ring, patch, pill come in that order is the ring, you have 12-13 times a year to mess up, the patch, you have 52 times a year you could mess up, and the pill, you have 365 times a year that you can mess up.
And then comes condoms. We always recommend condoms to prevent against sexually transmitted infections. Just assume everyone has every sexually transmitted infection under the sun, because 90 percent of people with chlamydia have no symptoms at all. A lot of people with HPV—make sure you get your HPV vaccine, if you haven’t gotten it—they have no idea that they have it, and then you have sex and then a couple weeks later you get HPV, I guess that person had HPV, so better safe than sorry.
And know that there are different thicknesses of condoms, and so at our teen clinic at Stanford, I pride ourselves in getting the best condoms with the best sensation, the thinnest condom without breakage, so that way you have a great experience and you’re more likely to use it.
And then withdrawal, a lot of people do use, but withdrawal is not the greatest method, and particularly for the one with the penis. Eventually the body will adapt and have premature ejaculation, which is an embarrassing kind of thing. But also as soon as the penis is erect, there’s some pre-ejaculate on there that has 10,000 sperm, and I ask people, how many sperm does it take to get pregnant? Just one! Though usually you need like 1,000 at least, but 10,000 sperm in the pre-ejaculate. So, as soon as penis is up, throw that condom on. Don’t do withdrawal, there’s a risk, but it’s all about whatever works for you, whatever is best, and what your risk tolerance is for getting pregnant.
So, there is a new patch out there and it’s called Twirla. Generally, as an academic, we don’t like to speak in name brands. What’s different about this one is it has levonorgestrel, whereas Xulane, the original patch, has a different progesterone in it.

The other thing is when they looked at Xulane and the blood levels of estrogen, it was more like a 50 microgram pill, whereas most films are 30-35 microgram, and so in general, doctors did not like the original patch because it was too high of a hormone, and so this patch was specifically made to have a lower, more acceptable hormone.
The negative is it’s $190 because it’s name brand versus $110. However, thanks to the Affordable Care Act, if you have insurance, your parents’ insurance or your personal insurance or even Medicaid, Medi-Cal, it should be covered with no copay, no deductible, because thanks to Obama and Biden, who passed the Affordable Care Act, that is the law that they passed—unless your employer is religious such as Hobby Lobby or the Catholic Church, or the Jesuit colleges like Georgetown, USC, Santa Clara University. The comparison is a standard birth control pill is $15 per month.
It’s not for people who have a BMI 30 or greater because number one, it doesn’t work so well, and number two, you’re at greater risk of blood clots.
So, the geek in me wanted to share this graph. The area under the curve is how much estrogen you’re exposed to, and the more estrogen you’re exposed to, the greater risk of blood clot.
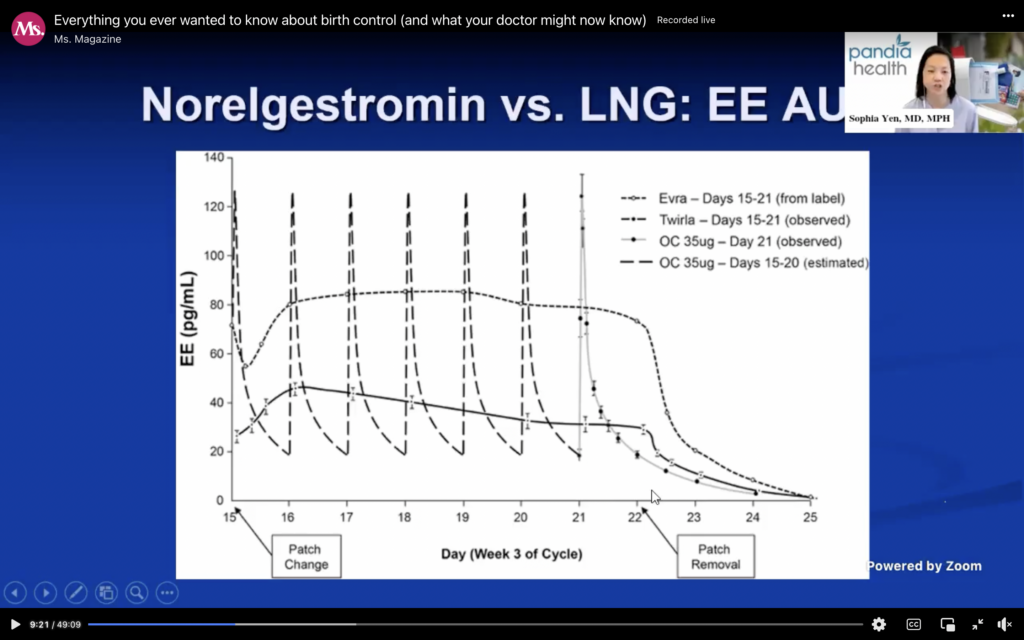
So, a 35 microgram pill here is up and down, up and down, up and down, but it doesn’t matter so much the up and down, but just the area under the curve, if you were to color this in, is how much estrogen you’re exposed to, and the original patch is up here, so you can see that’s a lot of estrogen you’re exposed to, and the new patch was developed to mimic the 30-35 microgram pill.
There’s a one-year vaginal ring, and when I first heard about it, I was like, this is amazing. It’s going to totally destroy the IUD/implant market because there’s a bunch of doctors that can’t do the IUD or implant, but certainly we can prescribe you a ring and you can just stick the ring up there for a year. So, you heard me right, you could just stick the ring up there for a year. What’s crazy is when they brought it to the United States, the FDA is like, well, can you test it where it’s three weeks in, one week out so that women can have an arbitrary bleed one week out of four? And they did, and it works, but know that it was originally tested abroad and it was tested for just leave it in for a year, so you absolutely could just leave it in for the year, but that’s off-label.
It has not been adequately evaluated in those with a BMI greater than 29. It’s effective, as effective as the pill/patch/ring in general. It does not require refrigeration. The negative is it’s expensive, $2,500, but as I mentioned before, if you have insurance, under the Affordable Care Act, it should be available with no copay, no deductible.
The negative of it is it only has 13 micrograms of estrogen, and as an adolescent medicine specialist, we generally recommend at least 30 micrograms of estrogen until you’re 30 years old. If you have less than 30 micrograms of estrogen, it’s not good for your bone density, and later when you’re 50-60-70, you’ll have a higher risk potentially of getting a fracture. So in general, whenever I give this talk, a bunch of people with uteri will turn over their birth control pill pack and be like, I’m on 20 micrograms of estrogen. So, if you’re under 30 and you’re on 20 micrograms of estrogen, it’s not good for your bones—so that’s your public service announcement or educational clinical pearl to take home today.
There’s a lot of talk of over-the-counter birth control, and of course I support all birth control pills going over the counter. The key to know is that not all pills are the same. There are 40 different birth control pills in there, and the one that has applied to go over the counter is a progesterone-only pill. The joke in medicine is: What do you call a woman who’s on a progesterone-only pill? You call her Mama or pregnant, because the progesterone-only pill with norethindrone in it, if you are late by three hours—you’re flying across the United States, you forget, you mess up your time zone, you stay out late at a movie or whatever like that—you need emergency contraception if you had heterosexual sex in the past five days and/or if you intend to have sex in the next three to five days. You need to have backup or abstain or use a condom as the hormone builds back up.
So, it’s not a very forgiving pill, but if you’re anal retentive and you can take the pill at the exact same time every day plus or minus two hours, then you’re good, but a lot of women have a hard time adhering to that regimen.
It is something that we generally give to breastfeeding women because if you give them a standard birth control pill with estrogen, that affects the breast milk in that it can decrease the production, so that’s why we also call women on the progesterone pill Mama, because they’re generally breastfeeding.
Know that I’m concerned that the progesterone-only pill is going over the counter. I think it absolutely should, but if people all like, “Oh, it’s over the counter,” and they go there, we could have a lot of pregnant people with uteri on our hands.
And then the next pill that’s up for going over the counter is a 20 microgram pill, and as I just said, if you’re under 30 years old, we don’t recommend less than 30 micrograms of estrogen for your bone health. However, if you’re a big-boned woman, you could probably get away with it—but for people who have a higher BMI, it’s actually better to be on a higher estrogen one, the standard estrogen, not the 20 microgram, because you need to get a certain level to prevent eggs from popping out and for the method to actually work.

So, top three reasons for missing a pill. Number one and two is forgot, away from home, no new pack. What can you do about it?
There’s an alarm. An acquaintance of mine has a birth control pill holder, so if you have the standard 4 by 7, you slip it in, and when you pop out a pill, it notes it. And if you don’t pop out a pill by a certain time at night, it will keep pinging you until you do. And then another one is an extra travel pack. Ask your doctor to give you some extra packs so you can have one in your travel. I always have one in my travel toiletry bag and then I carry one on-person because if my luggage gets stuck I don’t want to be literally screwed or bleeding when I don’t want to bleed.
And then know that as a doctor, I didn’t know that if I write dispense one, refill times 11 or 12, that I’m actually tying you to the pharmacy and forcing you to go every single month. A pharmacy cannot expand a doctor’s prescription, but they absolutely can constrict it. So, you can teach your doctor, “Dr. Sophia Yen at Stanford said that you can dispense 13 packs at a time, and if the insurance doesn’t cover it or whatever, they can shrink it, but if you’re okay with it, please dispense a year at a time”—and then 17 packs if you’re skipping the last week and skipping your monthly withdrawal bleed, because you’ll need more packs because you’re skipping.
And then lastly, delivery services.
So, now emergency contraception.
Going from left to right, left being most effective, right being least effective.
Number one is the copper IUD. The most recent study that did a head-to-head with the copper IUD and the levonorgestrel IUD standard dose 52 milligrams, showed zero out of 300-plus people that used the copper IUD for emergency contraception got pregnant. With the levonorgestrel, it was like three out of 313—and so the good news is if you were to show up in the ER and you needed emergency contraception, you could throw down a copper IUD and there’s almost zero chance of you getting pregnant.

So, if it were me, my daughter, my friend that was sexually assaulted and we wanted the lowest possible chance of being impregnated by a rapist, copper IUD. Most ERs, and particularly academic ERs, so like Stanford, UCSF or UPenn, any affiliate of a big hospital, can call an ob-gyn to come down and throw up a copper IUD.
Or for all of these methods, you technically have up to five days to use them, but if it were me, my friend, my daughter, my patient, my customer, I say if the condom pops at 3 a.m. in a heterosexual relationship, you want the medicine in that person with the uterus’s mouth by 3:10. No cuddling, huddling, snuggling, waiting till the morning after. ASAP, because as soon as the egg pops out, most of these methods will not work. However, I think the copper IUD will still work. The copper IUD is some strong stuff.
But I’m not a fan of the copper IUD because more blood, more cramps. So then you could throw down the hormonal IUD and then you’d have birth control for the next five to seven years—so know that that’s possible, and if you want the hormonal IUD as emergency contraception, you’re going to have to cite Dr. Sophia Yen or New England Journal of Medicine 2021.
And then there is Ella, and that’s the one that’s prescription only. So, Ella beats Plan B at every single time period, and if it were me, my daughter, my friend, and this is what we do at Pandia Health, we always recommend Ella, and the reason why is it beats Plan B at every single time point and it works up to a BMI of 35, so that’s hitting up on Plan B and its generics. It’s great, it’s over the counter, but if your BMI is 26 or greater—and that’s the PSA of the day, everybody please, go to a BMI calculator, calculate your BMI, and if it’s 26 or greater, Plan B and its generics don’t work so well for you, and if your BMI is 30 or greater, it doesn’t work at all. This is very important information that I ask all of you to please get out there to the public.
And then lastly, if you’re stuck in the middle of nowhere and all you’ve got is a bunch of birth control pills that have either levonorgestrel or norgestrel in it, generally you can take four pills now, four pills in 12 hours—but again, all these other ones are much better options, but if you’ve got nothing else and you’re alone and you can’t get to a doctor within the next five days to get whatever you need, then that is an option.
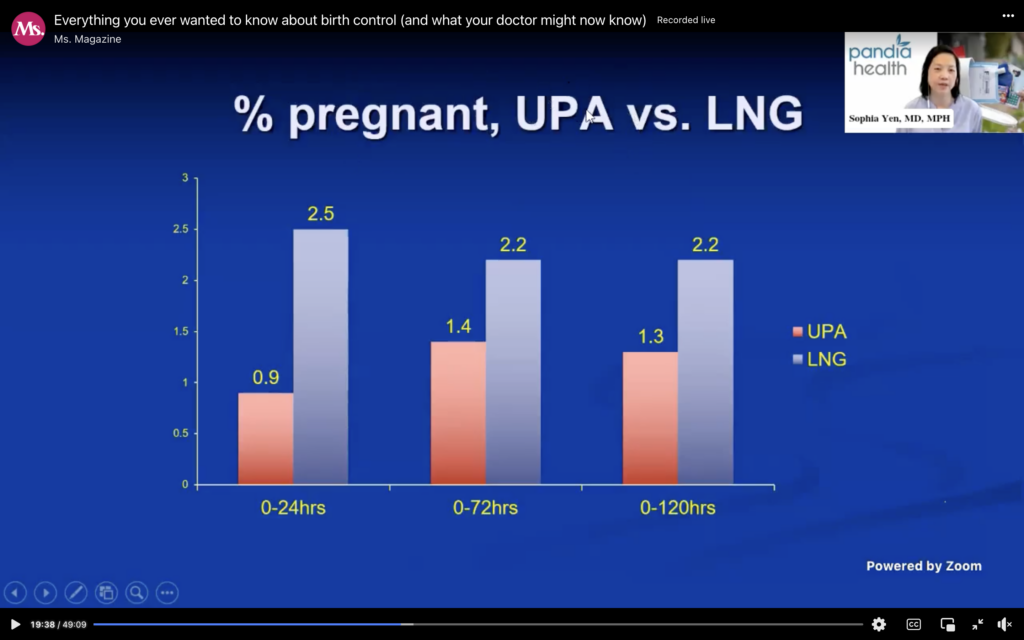
So, this is just showing you percent pregnant on UPA, which is Ella, versus levonorgestrel, which is Plan B, and Plan B has higher pregnancy rates at every single time point compared to Ella, and the other bonus about Ella is if your doctor writes for it, again, free. No copay, no deductible.
And then here’s just going over again, if your BMI is 26 or greater, which is about 147 pounds for five-foot-three, 176 pounds for five-foot-nine, the generic emergency contraception and Plan B are not so good, and if your BMI is 30 or greater, it doesn’t work at all. If your BMI is 35, then your only option is the IUD.

Get emergency contraception in advance.
And also discuss it with anyone with a penis, because if I were the person with the penis and my person is like, oh, crap, or I was like, oh, crap, the condom popped, I’d be like, I’m not going to say anything. I’ll stand by her side, and if anything happens, I’ll support her decision, but why be the bearer of bad news? But if you know about emergency contraception and be like, oh, the condom popped, and then you whip out your Plan B because you’re the one with the penis, and then the one with the uterus would be like, ha ha, I have some Ella, so that is the ideal world, but if those with penises don’t know about emergency contraception, they may not fess up when the condom pops.
If those with penises don’t know about emergency contraception, they may not fess up when the condom pops.
So you want emergency contraception just sitting in the corner waiting for the emergency to happen, because you want it there when you have a fire to put out the fire so you can save the situation. You don’t want it and you run to the pharmacy, it’s closed, the pharmacist won’t give it to you because against their religious belief, even though it doesn’t…levonorgestrel emergency contraception has no effect once the egg and sperm hooks up, has no effect on implantation, but who are you to go argue with the pharmacist at three AM, right? So, get it in advance of need.
We actually write on our prescriptions for Ella, please give the patient with the farthest expiration date, because otherwise they’ll give you the one that expires today.
And then as you choose online telemedicine, if it’s your doctor, go right ahead, but if it’s choosing between two online companies, make sure you know what’s good versus bad. Who is the CEO, founder, investors? Are they after you for money or are they more mission driven?
I like to say I’m the only CEO of a birth control delivery company that has taken the oath: Do no harm. Can’t say the same of the MBA people out there. Do they list their providers’ first and last name? Is there a lot of turnover and that’s why they don’t list anybody’s name? Are their providers doctors or nurse practitioners or PAs? Not to diss those people, but MDs have generally more training. How much training do they have? How many years?
Are they opt in or opt out? And for example, one company was like, I’m going to write this prescription for female condoms and I’m going to send it to your house unless you stop me, so generally not a good idea. More like, would you like some emergency contraception? Okay. This is the one we recommend. Okay. You’re good with that? We’ll bill your insurance. We’ll send it to you, but not I’m going to send this to you unless you tell me.
And then lastly, I love the generalists, but I’ve spent the past six years just focusing on birth control and that’s all I do, so I know how to manage the side effects, I know what works in one group versus another group. If they’re a generalist and they’re doing urinary tract infection and they’re looking in your nose and your ears, they may not know as much about birth control as somebody who only does birth control.
And then number seven, don’t call it birth control. Let’s make it “hormone therapy” to level the playing ground. There are a bunch of different reasons to use birth control not for birth control. Know that 70 percent of people on hormonal birth control pills are also using it for non-birth control reasons.
The medical community has done a great job drilling it in your head, you must bleed every month.
So, I thought I came up with the idea that you don’t have to bleed every single month, but I was wrong. Dr. Coutinho came up with it in 1999, but I’ll give you the background to understand.
I realized trying to get pregnant, the only reason those of us with uteri bleed is we build up that lining and we’re like, embryo? Oh, no embryo. Bleed. And then we build it up again? Embryo? No embryo. Bleed.
And as you all know, we get our first period at 12 and a half and we get our last period at 50. Why are we building up the lining? Every time you build up that lining, it can mutate and turn into endometrial or uterine cancer. Every time you pop out an egg, you risk ovarian cancer, and actually by being on the pill/patch/ring for five years, you decrease your risk of ovarian cancer by 50 percent.
So, people will then say, oh my gosh, but it’s not normal not to bleed every month, and yes, the medical community has done a great job drilling it in your head, you must bleed every month, and yes, if you’re in a first world country, have enough nutrition, and you’re two years after your first period, you should bleed every single month.
However, Dr. Beverly Strassmann, an anthropologist, studiess the Dogon tribe of Mali in Africa—and that’s not like centuries ago, it’s recently—and she studied them for 736 nights, and what she found, on the left, the Dogon women had 100 periods in their lives. In the United States, those of us with uteri have 350 to 400, so we have enough periods for three other people with uteri, and the reason for this, they start their periods later, 16, we start at 12. Basically when you hit 100 pounds or 22 percent body fat, you get periods because your body is like, oh, I have enough nutrition to support another being. And they have seven periods per year, we have 13, again, nutrition, but more importantly, they have eight or nine children.
How many periods you have when you’re pregnant? Zero. How many periods do you have when you’re exclusively breastfeeding every two to three hours? Zero. And so here, pregnant or breast feeding is the norm. Here, incessant menstruation is the norm. So, it is more natural to have fewer periods than what we are currently having.
So, better with stable hormones or no bleeds. Acne, arthritis, depression, diabetes, seizures. If you have painful or heavy periods or PMS or PMDD, if we get rid of your period, then we get rid of that problem. The number one cause of anemia in menstruating women is menstruation, and it can result in less ovarian, endometrial, colorectal cancer.
Every time you build up that lining, it can mutate and turn into endometrial or uterine cancer. Every time you pop out an egg, you risk ovarian cancer.
Just so you all know, the number one cause of missed school and work under the age of 25 is bad, evil periods. So, if you have bad, evil periods, please see a doctor. Please get treatment.
And know that environmental, it’s 10,000 to 13,000 tampons and pads.
If you’re not on any hormones or medications to stop your periods, you should have a period every month, mainly to make sure you don’t have pregnancy, thyroid, or tumor in your head, but know that we now have the technology to make periods optional.
I’ll stop there and have Roxy take it back.
Roxy Szal: Thank you, Dr. Yen. That was incredibly informative.
We heard about perhaps less well-known emergency contraception. Who knew that inserting a copper IUD after unprotected sex could prevent pregnancy better than Plan B? For me, that was kind of a game-changer when I heard that.
We also learned about the importance of knowing really who is prescribing your birth control and what are their motives and what is their background.
We talked about all the available birth control options, we talked about emergency contraception options, we talked about period options—or lack of a period—options. The importance of having abortion pills and emergency contraception in your medicine cabinet for a rainy day.

I’m getting some questions in the chat, so I’m just going to open up the floor now to have Dr. Yen answer some of your questions and so we can kind of process together what Dr. Yen just talked about.
Someone would like you to quickly clarify the difference between Plan B and Plan C.
Dr. Sophia Yen: So plan A is your normal, everyday birth control, and hopefully you chose a good one, like a long-acting reversible contraceptive or the one-year ring, or the pill, the patch, the ring, which aren’t as good as the longer acting ones.
Plan B is a euphemism for the entire emergency contraceptive class, which we talked that there are four different emergency contraception options. Know about the IUD, know about Ella, all of which beat Plan B and its generics.
And then Plan C is the new euphemism or the new cool, hip way to say medication abortion, and so medication abortion is mifepristone and misoprostol. Two pills. You take one of them now, and then, I believe 24 or 48 hours, you take the other four pills of one type in your cheeks, that’s called buccally, and you let it sit there for 30 minutes, and then whatever is left after 30 minutes you drink down, or you can do it intravaginally. Intravaginally has fewer side effects. However, if you’re in a state that’s hostile to reproductive rights, abortion rights, you might not want to put in your vagina because if you end up in the ER and they find the pills, then there might be an issue, but that’s just a tip.
Roxy Szal: Interesting, because I hear a lot of people, especially uninformed lawmakers, equating them all together and acting like they are abortifacients, so thank you for that.
Dr. Sophia Yen: Yeah, so follow up on that. If you’re pregnant and you take Ella, Plan B and its generics, or a bunch of birth control pills, nothing will happen. We don’t recommend doing it because just waste of money. Ella, theoretically, we don’t know what it could do, but at that dose, it probably doesn’t do anything.
If you have a positive pregnancy test, emergency contraception is not the answer. If you want to terminate, you need a medication abortion, Plan C, or you need a surgical abortion. If you have a positive pregnancy test, do not use emergency contraception. It will not work. It’s a waste of money.
Roxy Szal: Thank you. Okay. We have another question. How often can someone take emergency contraception and is there a limit to how many times you can take it, especially any health risks?
Dr. Sophia Yen: So, there is no health risks to taking emergency contraception every other day, though I wouldn’t recommend it. They are very jarring on your system, and the way that the Plan B and its generics works is it, like, tells the body you’re pregnant, and the body is like, oh, if I’m pregnant, I’m not going to pop out another egg, because then you’d have two pregnancies in your uterus at different times. So, that’s how that works.
If you’re taking emergency contraception more than once a month or twice a month, you should be on Plan A, not Plan B emergency contraception. Let’s get you on something that works 95-99 percent of the time versus emergency contraception, which works 75 or even lower.
Once the egg is popped out, often it’s too late and it won’t work at all.
Roxy Szal: I’m getting some questions in the chat about the effectiveness of diaphragms.
Dr. Sophia Yen: It’s kind of gone out of favor. It’s very rare because in the old days you had to go get it fitted. There is now a diaphragm that’s one-size-fits-all, but the negative of one-size-fits-all is if you’ve given birth then your cervix is a little bigger, and so it may not fit as snugly, and if it doesn’t fit snugly, then the sperm all run in, but yes, it’s definitely an option. It just isn’t as good as any of the hormonal. It’s more down towards the condom, withdrawal, fertility awareness method efficacy.
Roxy Szal: You touched on this towards the end of your presentation, and I think a lot of people are kind of curious. Your latest health campaign about educating the public about #PeriodsOptional. So, I’m getting a few questions so I’m just going to ask you kind of generally, you know, maybe you could speak on this for a minute or two. What do you wish people knew about skipping their periods?
Did you know that it’s completely safe to stop your period? It’s actually *safer* than having a monthly period, according to many health experts, like @teenmd of @PandiaHealth. #PeriodsOptional https://t.co/d0uFlJYuTg
— Ms. Magazine (@MsMagazine) April 24, 2020
Dr. Sophia Yen: One, that it is actually more natural to have fewer periods than we’re currently having. So, the take-home is we’re having 350 to 400 when it’s natural to have 100, and that by bleeding, building that lining up every single month, we risk endometrial, uterine cancer, and by popping out the eggs, we risk ovarian cancer. So, you actually decrease ovarian, endometrial and colorectal cancer by not having that withdrawal bleed every single month.
And so I’m a tiger Asian mom in Silicon Valley. I ask anybody with a child, with a uterus: Is your daughter going to do better bleeding or not bleeding on the SAT? In marching band? At that volleyball tournament? Playing soccer? Tennis in a white skirt?
The U.S. Women’s Soccer Team should talk to me because. I would make sure you don’t have any periods around the Olympics.
A Chinese Olympian as well, she came out of the pool and she’s like, oh, I think I lost a millisecond, and I was like, who’s your doctor? I bet you was a dude, because if it were me, I’d turn off your period.
I ask anybody with a child, with a uterus: Is your daughter going to do better bleeding or not bleeding on the SAT? In marching band? At that volleyball tournament? Playing soccer? Tennis in a white skirt?
Roxy Szal: We’re getting questions about abortion pills. You touched on Plan C, so we got a question: How easy is it to get Plan C through the mail in states where it’s illegal?
Dr. Sophia Yen: If you go to plancpills.org, you can get it on Aid Access, and it would be to make your period regular, and I would not check a pregnancy test, just if your period is not here then I would take it if you can afford $105 a pop, right? And I do think having it around, but you can also go to other states where it is legal, but we don’t know the legal ramifications of coming back and could they arrest you.
I’m not allowing my daughters to apply to colleges in any of the states where they are unfriendly and do not respect bodily autonomy, and we’re actually going to start a petition that petitions the governor of every state and the presidents of all the colleges, saying, you could have had this, my daughter, cool Asian American, kick-butt computer science major, but she’s not going to your state and she’s not going to marry and raise kids and grow in your state. You’re going to lose this opportunity, so you need to change your laws.
Roxy Szal: I just want to share anecdotally, I live in Texas and I ordered advanced provision abortion pills through plancpills.org. I was not pregnant, but I have them in my medicine cabinet if there’s a day that I am pregnant. Plan C wants to help. They have options like mail forwarding. You can get it mailed to a friend and have them mail it to you.
This is not legal advice. I’d love to plug the If/When/How hotline if you ever get yourself into some sort of legal trouble, but trust me, PlanCPills thinks it through.
Someone else asked, on the topic of abortion pills, if you could speak to the effectiveness of misoprostol alone, and is it easier to get?
Dr. Sophia Yen: It is easier to get in a Mexico or other countries, but in the United States, the pharmacists are starting to question even methotrexate. People are using methotrexate for rheumatoid arthritis, but because of this stigma, the pharmacists are afraid you’re going to use it for abortion, and I was like, how dare you withhold medicine for a health condition, any health condition, because you think I might use it for something else?
And so yes, misoprostol can be used to treat ulcers. I believe that for mifepristone, it can also be used to treat different cancers, and there’s a whole Feminist Majority Foundation background on that that’s amazing and so cool, but it’s not as effective. So, if you do mifepristone/misoprostol, I believe it’s like 92 effective done within the correct time period, and with misoprostol, it might drop to like 80-85, and so then you might need to go for surgical termination.
[Note: Study after study has found that self-managed abortion with misoprostol is more than 90 percent effective.]
Another key thing is if you walk into the ER, they can never turn you away. They have to take care of you, and also, if you didn’t stick it up your vagina and there are pills there, there is no way to tell the difference between a spontaneous abortion, which is a miscarriage, that is the medical term, spontaneous abortion, AKA miscarriage, or a medication abortion that started and didn’t finish. So, you can just walk in. You don’t have to say any, just like, I haven’t got my period and this happened, and let’s just go with spontaneous abortion.
Roxy Szal: Thank you. Quick question, what’s the shelf life of abortion medication? I believe it’s two years, right?
Dr. Sophia Yen: Yes, and same thing with Ella emergency contraception, and Plan B and its generics, so always ask for the one with the farthest expiration date. Make it clear to whatever pharmacy that are filling it so they don’t give you one that expires in the next month because they think you’re going to use it within the next 10 days or the next couple weeks. And then if you’re in the pharmacy, this is a very practical point, and you get it, do not walk out of the pharmacy. Look at the date immediately and be like, no, I want the one with the farthest expiration date, because once you walk out, you cannot return it. No pharmacy can take back drugs because they don’t know if you poked holes in it or dipped it in cyanide or something like that.
Roxy Szal: Thank you. Someone asked the question, if we go no periods, how do we know if we do get pregnant, especially if we are a teenager or in perimenopause?
Dr. Sophia Yen: You would have signs of pregnancy. You would have breast tenderness. That’s how I knew I was pregnant. I normally have no breast tenderness, but when I was trying to get pregnant, in the middle of night, at 3 a.m., bam, the boobs were like oh, and I was like, pee on a stick, pee on a stick, and I was pregnant. You would also have nausea. You would also have weight gain.
And then also know there have been women on the pill, women on Depo that were pregnant and it did nothing to the pregnancy, so be allayed, your concerns, that it would not affect the pregnancy. It would not turn it into a boy or a girl because of the hormones, would not mutate it or anything, but you should have pregnancy symptoms.
Roxy Szal: Okay. We have a lot of questions. ‘I use a period app to track my track my cycle for fertility awareness method. What alternatives to these apps should I use if I delete my app?’
Dr. Sophia Yen: So, I would say paper and pen and a cute little calendar. There’s so many cute little calendars out there you could buy. Also, make sure it’s a code that only you understand, in case somebody wants to tell on you.
My concern, you know, there are people that don’t like you. There are people that are jealous of you. There’s premeds that want to see you kicked out of the premed line. There’s a sorority sister who you spurned and she’s going to get back at you, and that’s the horror of what’s being done to this country, is we’re turning people on people, and the person who likes to tell on people, which I do believe in telling on bullies, but telling on somebody who’s taking care of their health, very different thing.
Roxy Szal: What about this question: What about the proven risks of pulmonary embolism, even with the patch, not the pill, in very young women?
Dr. Sophia Yen: That was probably with the 50-microgram pill and not with the new pill. With any estrogen-containing method, there is the risk of pulmonary embolism, there’s a risk of we call venous thrombus clots and all sorts of clots, and the acronym to remember is ACHES: abdominal pain, chest pain, headache, eyes, and swelling. So, if you get any of those, that could be a blood clot in that area.
So, I’d just recommend anytime you’re getting on a plane longer than three hours, take an ibuprofen or an aspirin before you go on, drink water and walk around, because more than three hours sitting, and you’re on an estrogen-containing thing, you are at a risk of blood clots.
Certainly if you have a strong family history of everybody getting blood clots, get tested, because if you have a blood clotting disorder, then that is a no-no for the birth control pill/patch/ring. Always disclose all of your medical history, but in general. and somebody under the age of 25, non-smoker, no blood clots running through their family, the benefits of birth control outweigh the risks.
Roxy Szal: Some people are asking, how can I hear more from you? And so maybe, Sophia, if you wanted to speak a little bit about how does Pandia Health work? And how can people stay in touch with what you’re talking about?
Dr. Sophia Yen:. Definitely follow Pandia Health on all of our socials. We have a ton of videos on YouTube, so if anybody needs sex ed resources, anything about the pill, patch, ring or emergency contraception, we got that on YouTube.
We also have, the second Tuesday of every month at 5 p.m. Pacific en español, and 5:30 in English, a Facebook live that we stream to YouTube and maybe Instagram as well. So, if you have a question, you can hit me up live the second Tuesday of every month except for when we have special speakers.
I’m happy to speak to employee groups, would love to speak to employee groups. Hit me up through, you know, either Facebook or Instagram, direct messaging, and say, I would love to talk to Dr. Yen, how big is the audience, I love Zoom because I don’t have to travel anywhere and I’ll do it for free if it’s 60 or greater people. Maybe I’ll start charging in the future.
And Pandia Health, I started it because I was giving that talk, why do women miss their birth control, and one of the top reasons was didn’t have it in their hand, and my friend and I were like, we’ll solve this. We’ll just ship you birth control, keep shipping it until you tell us to stop, and then we ran ads, free birth control delivery, 60 percent of the people that responded didn’t have a prescription, and it’s like, don’t you know in the United States you need a prescription? But I’m a doctor, I can write prescriptions, and thus Pandia Health was born.
We can deliver to all 50 states. If you have a prescription and insurance, you pay us nothing. Just tell us where it’s at, we move it to our pharmacy and we bill your insurance, we ship it to your door, and behind me you can see, every package comes with something delightful. We currently default to Hi-Chew, but we have a partnership with Winky Lux, we’ve given out lube, we’ve given out condoms, we’ve given out Cuterus stickers, all sorts of fun stuff, and then it also comes with the Pandia public service announcement, that postcard: Did you know about Plan B’s BMI limitations? Did you know you can use birth control to make #PeriodsOptional?
We ran ads, free birth control delivery, and 60 percent of the people that responded didn’t have a prescription. It’s like, don’t you know in the United States you need a prescription? But I’m a doctor, I can write prescriptions, and thus Pandia Health was born.
And then we can prescribe in 14 states, and we encourage birth control tourism, because it’s the major big states, so if you happen to be going to Vegas, happen to be going to any of the Disneys, if you happen to be going to Texas, New York, Pennsylvania, Georgia, Illinois and you fill out the questionnaire, give us a blood pressure from the past 365 days, 20 bucks once a year to use our expert doctors, and then unlimited follow-up questions about birth control, take advantage of it. Then we can ship it to all 50 states.
We take all private insurances. We definitely take California Medi-Cal and Family PACT, but we don’t take all the little Medicaids yet. We’re working on those contracts.
Roxy Szal: All right, y’all, I’m going to start to wrap this up.
In this post-Roe world, it’s becoming more and more essential for us to take charge of our reproductive health. This was an essential first step, and we hope we answered some of your questions and hope you took something meaningful away from this that you can apply to your life and share with your networks.
We at Ms. Magazine would love to stay in touch. The easiest way to do this is to head to our website and sign up for our weekly news alerts for MsMagazine.com, which is a place where feminists engage with each other and the world for action and social change, and where we cover reproductive justice, voting rights, and other issues on a daily basis.
Dr. Yen, any final words for our listeners?
Dr. Sophia Yen: Follow us everywhere @PandiaHealth, and if you want some crazy radical tweeting political, not associated with my employers and Pandia Health technically, follow me on Twitter @teenmd.
Follow Pandia Health, share Pandia Health, share #periodsoptional, pandiahealth.com/periodsoptional, and I also have Dr. Yen’s six tips now that Roe v. Wade has been overturned.
Roxy Szal: Thank you all so much for attending, and thank you, Dr. Yen, for being such a wealth of information. Talk to you all soon.
U.S. democracy is at a dangerous inflection point—from the demise of abortion rights, to a lack of pay equity and parental leave, to skyrocketing maternal mortality, and attacks on trans health. Left unchecked, these crises will lead to wider gaps in political participation and representation. For 50 years, Ms. has been forging feminist journalism—reporting, rebelling and truth-telling from the front-lines, championing the Equal Rights Amendment, and centering the stories of those most impacted. With all that’s at stake for equality, we are redoubling our commitment for the next 50 years. In turn, we need your help, Support Ms. today with a donation—any amount that is meaningful to you. For as little as $5 each month, you’ll receive the print magazine along with our e-newsletters, action alerts, and invitations to Ms. Studios events and podcasts. We are grateful for your loyalty and ferocity.
Up next:






